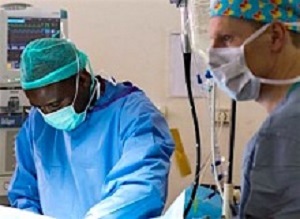
 In poor countries, like Rwanda, strep throat often goes undiagnosed and can lead to rheumatic fever and rheumatic heart disease, writes The New York Times. Since 2008, Team Heart has been annually flying in doctors to treat a fraction the patients needing their care in a country that has a collapsed healthcare system.
In poor countries, like Rwanda, strep throat often goes undiagnosed and can lead to rheumatic fever and rheumatic heart disease, writes The New York Times. Since 2008, Team Heart has been annually flying in doctors to treat a fraction the patients needing their care in a country that has a collapsed healthcare system.
The NYT writes that neighbours whisper that she is pregnant, a disgrace for a young, unmarried woman. The rumours mortify her. She hates her swollen belly. But Florence Ndimubakunzi is not pregnant. Her heart is failing. It pumps so poorly that blood backs up in her veins, bloating her liver and spleen, and filling her abdomen with fluid. She is only 18.
The report says for millions like her in poorer parts of Africa, Asia and other regions, this devastating heart disease began insidiously. During childhood, they contracted strep throat – an infection caused by streptococcal bacteria.
In the US and other rich countries, children with sore throats are routinely tested for strep and quickly cured with penicillin or other cheap antibiotics. But in poor countries, strep throat often goes undiagnosed and can become a long, slow death sentence. Without treatment, it can lead to rheumatic fever and rheumatic heart disease, in which the immune system attacks the heart valves – intricate flaps of tissue that must open and shut properly 100,000 times a day for the heart to work normally.
As the valves deteriorate, the heart struggles and gradually wears out. Patients become weak, short of breath and unable to attend school or work. Many die before they reach 30. Women with the illness who become pregnant can suffer severe and sometimes fatal complications.
The report says worldwide, 33.4m people had rheumatic heart disease in 2015, and at least 319,400 died from it – a public health disaster caused by a preventable disease that has been largely wiped out in the US and Western Europe.
Earlier this year, hoping to beat the odds, the report says Florence and her mother consulted doctors from a humanitarian group, Team Heart, that flies in from the US and Canada once a year to perform valve-replacement surgery. About 100 people showed up to be screened for the lifesaving operation. The team could operate on only 16.
Lying on an examining table, eyes huge in her gaunt face, Florence looked impossibly fragile, her arms thin as broomsticks, her shoulders jutting up like a skeleton’s. She had wasted away to 78 pounds; five were fluid. Dr Pat Come, a Harvard cardiologist, pressed a stethoscope to Florence’s chest, back and neck, and palpated her belly. A sonographer, Marilyn Riley, from Beth Israel Deaconess Hospital in Boston, ran an ultrasound probe over Florence’s chest, showing her heart valves in motion and measuring the pressure gradients across them, the blood flow through her heart and the size of its chambers. “She has significant disease of two valves,” Come finally said. “But the operative mortality is likely too high. Medical therapy is the best option.”
A translator explained in Kinyarwanda that Florence was too sick for surgery. Florence asked if the medicines would cure her. No, but they could keep her “on an even keel,” Come said. Would her big belly go away? Florence asked. A drug, Lasix, that helps rid the body of excess fluid might help, Come said.
As Florence sat up, buttoning her dress, Riley said, “She’s so tiny I’m afraid she’ll fracture getting off the table.” A nurse helped her down. Outside the examining room, Florence said she’d had to stop attending school because she was too weak to get there. She was eager to go back. She hoped to be a paediatrician. She has been ill since she was about 8. Doctors warned that only surgery could cure her. Now, they were saying it was impossible. “It’s a disappointment,” Florence said.
Experts say programmes to educate people about sore throats and strep, and to distribute penicillin widely to local clinics, could help greatly to prevent rheumatic heart disease in poor regions. But even those efforts probably would not wipe it out completely, because not everyone with strep seeks medical attention.
The report says the World Heart Federation, which works with the World Health Organisation, calls rheumatic fever and the heart damage it causes “neglected diseases of marginalised communities.” Poverty, crowded living conditions and lack of medical care create breeding grounds for strep. In 2013, the federation set a goal of decreasing deaths from the condition by 25% in people under 25 by 2025. The group also called for a strep vaccine.
The report says little is spent on studying the illness, less than $1m globally in 2013. From 500 to 1,000 times as much research money is spent on tuberculosis, malaria and HIV – which each kill three to five times as many people as strep, statistics say.
If rheumatic fever is detected early, long-term treatment with penicillin can prevent valve damage. But, the report says, many cases are already advanced. “Unfortunately, the entry point is heart failure,” said Dr Joseph Mucumbitsi, a paediatric cardiologist at the King Faisal Hospital in Kigali, and a consultant to Team Heart. “We have many rheumatic heart disease patients below 17. We have some as young as 5.” He estimated that there might be as many as 20,000 people with advanced disease who need surgery.
Though prevention would be ideal, the report says the rapid tests widely used in the US to diagnose strep are too expensive in Rwanda, and throat cultures are not widely available. Some doctors advocate skipping the tests and just giving penicillin shots to all children with sore throats. Others worry that antibiotic resistance and penicillin allergies would result.
The genocide that killed 1m people in Rwanda in 1994 also destroyed its health care system, and the country has had to rebuild it. The report says HIV, malaria, tuberculosis and rotavirus have been major priorities – not heart disease. Rwanda has only five cardiologists and no heart surgeons or hospitals equipped to perform heart surgery – for a population of 12m.
The report says since 2008, Team Heart has been traveling to Rwanda. The group was founded by Cecilia Patton-Bolman, an intensive-care nurse, who had seen a ward full of teenagers dying from rheumatic heart disease when she visited the country in 2006, and her husband, Dr R Morton Bolman III, who was the chief of cardiac surgery at Brigham and Women’s Hospital in Boston. (He later moved to the University of Vermont, and recently retired.)
Once a year, 40 to 60 volunteers fly to Kigali: heart surgeons, cardiologists, nurses, anaesthesiologists, experts in cardiac ultrasound, biomedical technicians, pharmacists, support staff and perfusionists who run the heart-lung machine that keeps patients alive during surgery. They come from the University of Vermont, Harvard-affiliated hospitals and other medical centres. They pay their own airfare, and Rwanda’s Ministry of Health covers some hotel rooms and meals. Most use their vacation time, and this year Team Heart asked each volunteer also to raise $500 in donations to help cover costs. The doctors and nurses became so close to the patients that they routinely referred to them by first names in their private interactions and group deliberations, a practice reflected in the first-name references to the patients in this article.
A week before the operations were to begin, at the King Faisal Hospital in Kigali, Team Heart members visited other medical centres to screen patients. Riley, the sonographer, said, “The first year I came, it felt like ‘Who gets the life jacket in a sinking boat?’” The ideal candidates are sick enough to die in a year without replacement valves – but well enough to survive the operation. The screeners also rule out those who seem strong enough to wait another year. “Last year, we deferred someone who was too early,” Come said. “Then this year, he was too late.”
One year, a patient was turned down because she was pregnant, Come said. She returned a few days later – after an abortion. She underwent the surgery and did well.
[link url="https://www.nytimes.com/2018/09/16/health/rwanda-strep-heart-disease.html?nl=top-stories&nlid=71899860ries&ref=headline"]The New York Times report[/link]
