 Post-partum placenta ingestion is potentially harmful with no documented benefit, so physicians should discourage the practice, according to a research review in the American Journal of Obstetrics and Gynaecolology. There is no professional responsibility on clinicians to offer placentophagy to pregnant women following the celebrity fad.
Post-partum placenta ingestion is potentially harmful with no documented benefit, so physicians should discourage the practice, according to a research review in the American Journal of Obstetrics and Gynaecolology. There is no professional responsibility on clinicians to offer placentophagy to pregnant women following the celebrity fad.
Young celeb mothers from the US tell us in social and other media in which way they have eaten the placenta of their baby. On many esoteric and alternative medical websites you can also find instructions and even cooking recipes for the preparation of the allegedly healthy placenta.
This tissue rejected after birth is currently stylised as a superfood in a mixture of mythological and pseudo-medical arguments. Due to its high levels of nutrients and hormones, it is said to improve the milk production of breastfeeding mothers, to have a preventive effect against puerperal depression and to bring new energy and a faster recovery after pregnancy. However, none of the alleged effects are scientifically proven. On the one hand, because it would be ethically unacceptable to analyse this topic in a sufficiently good study design and, on the other hand, because an above-average placebo effect is to be assumed.
Gynaecologist Alex Farr from the Medical University of Vienna worked in cooperation with the Weill Cornell Medical Centre at the New York Presbyterian Hospital in New York and did research on the subject, which in some cases still is highly taboo. He recently published his findings as an expert statement.
Farr said: "Medically speaking, the placenta is a waste product. Most mammals eat the placenta after birth, but we can only guess why they do so. After the placenta is genetically part of the newborn, eating the placenta borders on cannibalism.”
Farr also sees no evidence of medical benefits. On the contrary, the presumed nutrients such as iron, selenium and zinc are not present in sufficient concentrations in the placenta. However, high concentrations of heavy metals in the placenta were found to accumulate there during pregnancy."
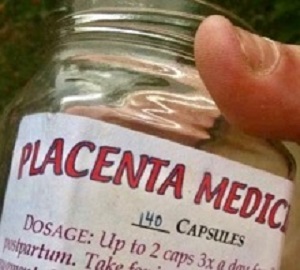
And above all, the consumption, which usually takes place in the form of processed capsules or globules, also carries a risk of infection.
Farr said: "It was not until June 2017 that the US Federal Department of Health, the Centre for Disease Control and Prevention (CDC), officially warned about this trend because of a recent case. The baby of a mother who had eaten placenta capsules suffered life-threatening blood poisoning from streptococcus several times. These bacteria could be detected in the placenta capsules of the mother and were probably transmitted by her to the child.”
The gynaecologist regards it as a problem that meeting the women's desire to take the tissue with them is a legal grey area. This can only be clearly prohibited if follow-up examinations of the placenta seem to be required from a medical point of view. Farr advises to strongly point out the risk to young mothers.
Abstract
Placentophagy or placentophagia, the postpartum ingestion of the placenta, is widespread among mammals; however, no contemporary human culture incorporates eating placenta postpartum as part of its traditions. At present, there is an increasing interest in placentophagy among postpartum women, especially in the United States. The placenta can be eaten raw, cooked, roasted, dehydrated, or encapsulated or through smoothies and tinctures. The most frequently used preparation appears to be placenta encapsulation after steaming and dehydration. Numerous companies offer to prepare the placenta for consumption, although the evidence for positive effects of human placentophagy is anecdotal and limited to self-reported surveys. Without any scientific evidence, individuals promoting placentophagy, especially in the form of placenta encapsulation, claim that it is associated with certain physical and psychosocial benefits. We found that there is no scientific evidence of any clinical benefit of placentophagy among humans, and no placental nutrients and hormones are retained in sufficient amounts after placenta encapsulation to be potentially helpful to the mother postpartum. In contrast to the belief of clinical benefits associated with human placentophagy, the Centers for Disease Control and Prevention recently issued a warning due to a case in which a newborn infant developed recurrent neonatal group B Streptococcus sepsis after the mother ingested contaminated placenta capsules containing Streptococcus agalactiae. The Centers for Disease Control and Prevention recommended that the intake of placenta capsules should be avoided owing to inadequate eradication of infectious pathogens during the encapsulation process. Therefore, in response to a woman who expresses an interest in placentophagy, physicians should inform her about the reported risks and the absence of clinical benefits associated with the ingestion. In addition, clinicians should inquire regarding a history of placenta ingestion in cases of postpartum maternal or neonatal infections such as group B Streptococcus sepsis. In conclusion, there is no professional responsibility on clinicians to offer placentophagy to pregnant women. Moreover, because placentophagy is potentially harmful with no documented benefit, counseling women should be directive: physicians should discourage this practice. Health care organizations should develop clear clinical guidelines to implement a scientific and professional approach to human placentophagy.
Authors
Alex Farr, Frank A Chervenak, Laurence B McCullough, Rebecca N Baergen, Amos Grünebaum
[link url="https://www.meduniwien.ac.at/web/ueber-uns/news/detailseite/2017/news-im-oktober-2017/gefaehrlicher-trend-plazenta-eignet-sich-nicht-als-superfood/"]Medical University of Vienna material[/link]
[link url="http://www.ajog.org/article/S0002-9378(17)30963-8/fulltext"]American Journal of Obstetrics and Gynaecology abstract[/link]
