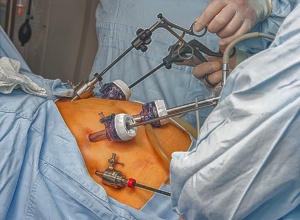
Responding to growing body of evidence pointing towards obesity as a major risk factor for coronavirus, there have been calls for a rapid expansion in NHS-funded weight loss surgery in the UK.
The Daily Telegraph reports that in a study of nearly 17,000 COVID patients in UK hospitals, those who were obese – with a body mass index (BMI) of more than 30 – had a 33% increased chance of dying compared to those who were not obese.
Another study found that nearly three-quarters (73%) of COVID patients in intensive care were either overweight or obese, compared to 64% in the UK population.
The report says frightened by the pandemic, many are now looking to lose weight fast – and surgery seems like a convenient fix.
Doctors have called for a rapid expansion in UK National Health Service (NHS)-funded weight loss surgery to lessen the impact of COVID over the next year or two, before scientists develop a vaccine. They hope their message will fall on receptive ears in Downing Street, where Boris Johnson reportedly told colleagues that he is preparing a “more interventionist” drive against obesity, following his own brush with the virus last month. The prime minister is said to have become convinced that his weight is the reason he ended up in intensive care while his colleagues suffered only mild symptoms – 17.5 stone, Johnson’s BMI is around 36, well above the threshold for obesity.
For NHS surgery, a patient needs a BMI of 40 or above; or a BMI of 35 or above with an obesity-related illness like diabetes or heart disease. Options include a gastric band surgery, in which a rubber ring is placed around the top of the stomach, helping to soothe a patient’s hunger; a sleeve gastrectomy, in which 80 percent of the stomach is removed, leaving just a thin ‘sleeve’ through which food can pass; and a gastric bypass, in which the stomach is ‘short-circuited’.
It is a major operation, and patients are advised that in a very small number of cases they might be left with gallstones or a blood cot in the leg, or with extra folds of skin, which might require extra surgery to remove. But most patients recover within a few days, doctors say. Those who do not want surgery can take a gastric balloon – a tablet which inflates inside a patient’s stomach, preventing them from feeling hungry. It starts to deflate after four months.
Professor David Kerrigan, president of the British Obesity and Metabolic Surgery Society, says his private clinic, Phoenix Health, now receives about 50 enquiries a week despite doing no advertising – “definitely far more than we normally would”. “It’s been looked at by the National Institute for Health and Care Excellence (NICE) and it’s one of the cost-effective treatments there is,” he says. “It works, and the UK is one of the safest places in the world to have bariatric surgery.”
Shaw Sommers, a consultant bariatric surgeon, says his private clinic has also seen a sharp increase in enquiries during the COVID pandemic. He thinks the NHS’s focus on preventative measures like diet and exercise does little to help the very fattest of patients, with a BMI over 40, for whom “you can diet all you like, your body’s just going to go straight back as soon as you take your foot off the brake”. He says that surgery also makes financial sense, with obesity and its related illnesses costing the NHS about £4.3bn each year.
But, the report says, not all doctors are convinced. With 27% of English adults classed as obese (and similar figures in the UK’s other nations), any attempt to expand weight loss surgery would heap further pressure on an already-burdened NHS budget. Some believe it makes more sense to plough that money into a mass preventative programme, including free weight loss classes for all overweight adults. In 2014, a group of surgeons criticised NHS plans to expand weight loss surgery as “nonsensical”, and Diabetes UK said it is the right option only for “a very small number” of patients.
[link url="https://www.telegraph.co.uk/health-fitness/body/nhs-funded-weight-loss-surgery-really-quick-fix-coronavirus/?WT.mc_id=e_DM1251908&WT.tsrc=email&etype=Edi_FPM_New_ES&utmsource=email&utm_medium=Edi_FPM_New_ES20200601&utm_campaign=DM1251908"]Full report in The Daily Telegraph[/link]