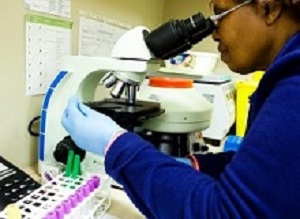
 Part of the research at the University of Cape Town's new new Aerobiology TB Research Facility involves measuring the amount of air individuals exchange, which may range from about 300 litres per day between children and adolescents, to 1,000-2,000 litres per day in places like Pollsmoor Prison.
Part of the research at the University of Cape Town's new new Aerobiology TB Research Facility involves measuring the amount of air individuals exchange, which may range from about 300 litres per day between children and adolescents, to 1,000-2,000 litres per day in places like Pollsmoor Prison.
At the age of five, 20% of children in Masiphumelele are already infected with tuberculosis (TB). When these children enter high school, about half are infected with TB. By the time they become young adults, the infection rate has increased to roughly 80%. That’s the reality for the community of over 23 ,00 residents in the heart of Cape Town’s “deep south”, home to the University of Cape Town’s (UCT) Desmond Tutu HIV Foundation (DTHF) Masiphumelele research site. Known commonly as the “Masi site”, it is also now home to the new Aerobiology TB Research Facility, officially launched on 20 February, which will focus on the study of the transmission of these TB organisms with a view to finding ways to halt the spread of the disease.
While these percentages relate specifically to research in Masiphumelele schools, there is nothing to suggest that this community is exceptional. Rather, the figures are an indicator that similar TB infection results will likely be recorded in township schools throughout the Western Cape.
Emeritus Professor Robin Wood, CEO of the DTHF and director of the Desmond Tutu HIV Centre (DTHC), an accredited research centre within UCT’s health sciences faculty, said at the launch that poor socio-economic conditions are one of the big drivers of TB transmission.
Research shows that the triple challenge of poverty, inequality and unemployment is most pronounced in townships in South Africa. “So, we have a major burden of TB,” said Wood, who is also a full member in UCT’s Institute of Infectious Disease and Molecular Medicine (IDM).
He explained that researchers at the new facility specialise in capturing the organisms in the air exhaled by patients, and “putting (the data) on to matrices which we can then look at very carefully.” This allows clinicians and scientists to study each individual organism to try and develop ways in which to control TB in communities such as Masiphumelele.
Part of the research involves measuring the amount of air individuals exchange with each other, for example. Wood said he exchanges about 25 litres a day whereas the children and adolescents studied swap approximately 300 litres per day. In a place like Pollsmoor Prison, Wood estimates swapping is between 1,000 and 2,000 litres per day.
“And that increases the chances of disease being transmitted,” he explained, adding that the centre researchers are effectively measuring the number of organisms in the air that are being exchanged.
Professor Linda-Gail Bekker, deputy director at the DTHC, chief operating officer at the DTHF and a member of the IDM, said at the launch there is a 20-year relationship between clinicians, scientists and the Masiphumelele community. The relationship dates back to 1999 when the staff at the Desmond and Leah Tutu Clinic began providing HIV care to Masiphumelele residents. That clinic is still situated in the community.
They then raised funds to build a dedicated research clinic, the Desmond and Leah Tutu Research Centre, adjacent to the public clinic. This was opened in 2004 – the year that the DTHF was established and opened at UCT’s faculty of health sciences campus. In 2011 an adjacent youth centre was built, providing upwards of 4,000 young people with a space to hang out, eat, read and access the internet.
Bekker also conveyed “support and love” from DTHF and DTHC patron Anglican Archbishop Emeritus Desmond Tutu and his wife Leah Tutu. “He is our role model for the work we do,” she said.
While the launch was about the facility and the work it will enable, it was also a celebration of interdisciplinary research, and IDM director Professor Valerie Mizrahi spoke of working with “giants in the field of medical research” like Bekker and Wood.
She praised Wood for his leadership, saying that as a polymath he understands the many fields at work, and is never intimidated by what he doesn’t know. This kind of leadership, she said, is key to interdisciplinary and now transdisciplinary research on the TB project.
“We are actually creating and pioneering new science here in Masiphumelele … new science, the aerobiology of tuberculosis that brings together state-of-the-art single cell microbiology. “There’s a merging of social responsiveness and basic research. It brings these together, making it impossible to distinguish (between them).”
UCT vice-chancellor and guest of honour Professor Mamokgethi Phakeng cut the red ribbon, officially opening the facility. She told guests the occasion made her extremely proud, first off because of what the facility will be able to do in the fight against TB.
“Imagine a future where we can talk about Masi as a place where TB used to be a problem,” she said.
She also praised the “friendship that has grown” between researchers and the communities of Masiphumelele and Ocean View. “The people of Masi and Ocean View have helped us in many ways. I want to acknowledge the important role (they) have played in … shaping the way we work here and how this work reaches different individuals and families.”
Commending her colleagues at the DTHF for their attention to community needs, Phakeng said UCT increasingly recognises that the “university lives in the community and the community lives in the university”. “It’s in moments such as this one that I wish I could call all of South Africa to come and witness … what we mean when we say the work that we do responds to the context that we live in. We are not just the best on the continent; we work hard to be the best for the continent.”
Addressing the DTHC, DTHF and IDM teams, she added: “You didn’t come to Masiphumelele because it’s fashionable. You were driven by the questions that you wanted answers to, and the questions that you wanted answers to are pertinent to the continent.”
The new research facility aims to curb TB by studying how it is transmitted in the local community. The Scientist reports that the R10m facility will allow microbiologists from UCT to study Mycobacterium tuberculosis captured from the exhaled air of local TB patients. It will do so using locally developed technology.
On the ground floor of the two-story building, TB patients will enter into a “clean box” about the size of a phone booth and spend some time in there. The air in the box – about 300 litres – will be vacuumed up and run through sterile water, locking any particulate matter including bacteria in a 5ml tube. Scientists will then scour the samples for TB bugs.
For now, it’s not the easiest or cheapest way to identify TB infection. But in time, the scientists hope to scale it up into a high-throughput diagnostic tool to help identify so-called “super-spreaders” in the community. They also want to identify the locations in the community where TB is spread, which would help target TB prevention services. “We want to find everyone who is transmitting in the neighbourhood,” says Wood.
The report says spotting super-spreaders will be easier said than done. To do that, the technology will have to be able to screen dozens of patients per day in Masiphumelele alone, returning findings quickly and without inconveniencing patients. This will require advanced automation of the sample processing, whereas microscopists currently have to inspect thousands of nanowells one-by-one to detect bugs in one sample. Research is also needed into whether the amount of TB a person exudes determines how infectious he or she is, or whether it’s specific strains of TB that drive infection.
Further afield, the challenge will be multiplied thousand-fold. The report quotes Wood as saying the city of Cape Town has more individuals living with TB than the US, the UK, Germany, and France put together and the bacterium infects twice as many people in Cape Town as it did 100 years ago. Childhood infection rates are particularly high.
The report says infection rates are so high here partly because HIV has rendered millions of South Africans susceptible to TB. But Wood thinks HIV alone doesn’t explain the elevated infection rates in places like Masiphumelele. Rather, he thinks there is a large reservoir of infected individuals who aren’t reached by treatment programmes, which focus on active disease. “You’ll never stop the disease unless you stop people getting it,” he says.
This is where the clean-room sampling technology comes in. Unlike TB tests where patients are asked to cough, samples from the clean box are passive – patients may cough if they need to (and these are documented), but they are not prompted to. This will allow the scientists to determine whether coughing transmits TB better than just breathing the same air as somebody who is infected.
The report says the technology is still in its infancy, and for the next few years, microbiologists from UCT plan to perfect the clean box collecting mechanism. Digby Warner from UCT’s Institute of Infectious Disease and Molecular Medicine who leads the microbiology work says it’s exhilarating to work on TB obtained from patients. Working on lab strains is “like seeing lions in the zoo,” he says. But studying TB from people infected naturally is “like seeing the organism in the wild.”
For others on the team, the centre’s location provides a welcome human connection with the disease they study. Anastasia Koch, who will study the genomic fingerprints of M. tuberculosis extracted from the samples, says she knows of no other location in the world where such high-tech equipment is located in such close proximity to the affected community. “That changes the way you think about the research,” she says. “As you drive into ‘Masi’ you think about how transmission happens socially. As basic scientists we don’t do a lot of social research, we don’t understand the social factors. But when you bring all of it together in one place, it becomes really powerful.”
The report says the next step for the microbiology team is to ensure that what they are seeing in the samples is, in fact, M. tuberculosis. To do that, they have to isolate single cells and study them – something the team hasn’t been able to do just yet. “We have a lot of circumstantial evidence that what we’re seeing in our slides is TB. It looks like TB, we can culture TB from it, and it stains like TB,” Warner says. But there’s a lot of “gunk” in the slides, including other bacteria, he says, and it’s vital for the sake of future automation that the TB identification is above reproach. “The challenge over the next few years is to get to a point where we can capture the organism off the slide, and either grow it up in culture or get a lipid or protein signal to confirm that what we have seen is definitely TB.”
For this next stage, the report says, Warner and his colleagues are teaming up with colleagues at Massachusetts Institute of Technology (MIT) and Imperial College London. They will use a new fluorescent probe developed by MIT to see if it is better at selectively labelling M. tuberculosis than the TB-highlighting probe the Cape Town team currently uses, called DMN-trehalose, and work on ways to extract the highlighted bacteria from the samples for further analysis.
But, the report says, Wood’s method of studying transmission is not without its detractors. Not all TB particles detected in exhaled air are able to cause infection, says Edward Nardell of Harvard Medical School, and counting microbes in the air could therefore overestimate the infectiousness of patients. Nardell is part of a group that since 2005 has been studying TB transmission in another part of South Africa by venting air from tuberculosis patient rooms through guinea pig cages to find how many animals catch the disease. “This measures actual infection, the event of interest,” he says. “Sometimes old methods remain the best.”
Eric Rubin, a microbiologist at Harvard TH Chan School of Public Health, says the work Wood is undertaking is “unusual and difficult.” But he says that while the transmission work on guinea pigs has yielded interesting and clinically translatable results, “Robin’s work is different as he is interested in underlying molecular mechanisms.”
Others are more unequivocally supportive, the report says. “Having such a dedicated unit unravelling how TB is specifically conveyed from an infected person to a susceptible person is a step change,” says Derrick Crook, an infectious disease microbiology specialist at the University of Oxford. “The benefit is that the factors that promote or prevent this can now be disentangled. Doing it where such spread is happening gives the researchers the best possible chance of sorting this out.”
[link url="http://www.health.uct.ac.za/news/pioneering-‘new-science’-masiphumelele"]University of Cape Town material[/link]
[link url="https://www.the-scientist.com/news-opinion/lab-in-south-african-township-to-sample-tb-from-breathed-air-65579"]The Scientist report[/link]
[link url="https://www.news.uct.ac.za/article/-2019-02-26-uct-launches-aerobiology-tb-research-facility-in-masiphumelele"]Video link[/link]
