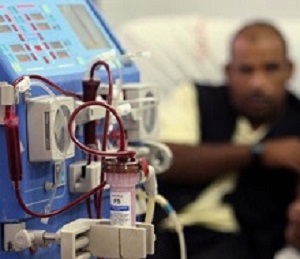
 Up to one-fourth of adults in sub-Saharan Africa suffer from chronic kidney disease and only a small fraction ever reach a dialysis treatment centre, a Swiss study has found.
Up to one-fourth of adults in sub-Saharan Africa suffer from chronic kidney disease and only a small fraction ever reach a dialysis treatment centre, a Swiss study has found.
Of those who did begin dialysis, most quit, usually within two weeks, because they could not afford to continue, and 88% died, the research found. Quitting dialysis almost always proved fatal.
“Among those who do manage to scrape together enough money to begin dialysis, the majority cannot afford to continue to pay for dialysis and die within weeks of starting, very likely after having depleted their family’s resources,” senior author Dr Valerie A Luyckx of the University of Zurich, Switzerland said.
The report said Luyckx, a kidney specialist who also studies biomedical ethics, worked on the study with colleagues in Cameroon, Ghana, Senegal and South Africa. Together they reviewed 68 previous studies covering nearly 25,000 adults and more than 800 children.
The found that 59% of the adults and 49% of the children stopped life-saving dialysis treatments for financial reasons, despite needing to continue. The high attrition rates raise ethical questions about whether healthcare workers should present dialysis as an option to patients who cannot afford it, Luyckx and her colleagues said.
In most sub-Saharan countries, patients must pay out of pocket for dialysis, she said. She described the costs as “prohibitive” and “catastrophic” because they “likely plunge families further into poverty.” Of those who needed dialysis but failed to receive it, 96% of adults and 95% of children died.
Only about 10% of adults and 35% of children with end-stage kidney disease remained on dialysis for three months, the study found. For people with this condition, the only alternative to dialysis that would allow for survival is a kidney transplant.
The report says in an accompanying editorial, Dr Ikechi G. Okpechi called the findings “alarming and outrageous” and said they should motivate policymakers to address care for those with end-stage kidney disease in the region. But “I have doubts that these data will influence those in government in sub-Saharan Africa,” wrote Okpechi, a kidney specialist at Groote Schuur Hospital and University of Cape Town in South Africa.
The government of Nigeria recently agreed to pay for the first two weeks of dialysis, Okpechi said. However, he added, “Such small, albeit positive, steps are a drop in the ocean.”
"(The study’s findings) make a strong case that there is an ethical imperative for governments to acknowledge the dire consequences of the lack of policies which lead to inequitable access to dialysis,” Luyckx said.
As many as 23% of adults in sub-Saharan Africa have chronic kidney disease, and up to 3m people die every year because they lack access to dialysis, her team writes. If treatment for end-stage kidney disease is unaffordable, “adequate palliative care options should be in place such that patients don’t disappear or abscond from hospital to die, likely often humiliated because they cannot pay,” Luyckx said.
“Like for HIV/Aids,” Okpechi writes in the editorial, “countries in sub-Saharan Africa should stop burying their heads in the sand and realise that the burden of (end-stage kidney disease) will worsen and every small step taken in the right direction now will help to save lives in the future.”
Abstract
Background: The burden of end-stage kidney disease (ESKD) in sub-Saharan Africa is unknown but is probably high. Access to dialysis for ESKD is limited by insufficient infrastructure and catastrophic out-of-pocket costs. Most patients remain undiagnosed, untreated, and die. We did a systematic literature review to assess outcomes of patients who reach dialysis and the quality of dialysis received.
Methods: We searched PubMed, African Journals Online, WHO Global Health Library, and Web of Science for articles in English or French from sub-Saharan Africa reporting dialysis outcomes in patients with ESKD published between Jan 1, 1990, and Dec 22, 2015. No studies were excluded to best represent the current situation in sub-Saharan Africa. Outcomes of interest included access to dialysis, mortality, duration of dialysis, and markers of dialysis quality in patients with ESKD. Data were analysed descriptively and reported using narrative synthesis.
Findings: Studies were all of medium to low quality. We identified 4339 studies, 68 of which met inclusion criteria, comprising 24 456 adults and 809 children. In the pooled analysis, 390 (96%) of 406 adults and 133 (95%) of 140 children who could not access dialysis died or were presumed to have died. Among those dialysed, 2747 (88%) of 3122 adults in incident ESKD cohorts, 496 (16%) of 3197 adults in prevalent ESKD cohorts, and 107 (36%) of 294 children with ESKD died or were presumed to have died. 2508 (84%) of 2990 adults in incident ESKD cohorts discontinued dialysis compared with 64 (5%) of 1364 adults in prevalent ESKD cohorts. 41 (1%) of 4483 adults in incident ESKD cohorts, 2280 (19%) of 12 125 adults in prevalent ESKD cohorts, and 71 (19%) of 381 children with ESKD received transplants. 16 studies reported on management of anaemia, 17 on dialysis frequency, eight on dialysis accuracy, and 22 on vascular access for dialysis
Interpretation: Most patients with ESKD starting dialysis in sub-Saharan Africa discontinue treatment and die. Further work is needed to develop equitable and sustainable strategies to manage individuals with ESKD in sub-Saharan Africa.
Authors
Gloria Ashuntantang, Charlotte Osafo, Wasiu A Olowu, Fatiu Arogundade, Abdou Niang, John Porter, Saraladevi Naicker, Valerie A Luyckx
[link url="http://www.reuters.com/article/us-health-dialysis-africa-idUSKBN16G330"]Reuters Health report[/link]
[link url="http://thelancet.com/journals/langlo/article/PIIS2214-109X(17)30057-8/fulltext"]The Lancet Global Health article summary[/link]
[link url="http://thelancet.com/journals/langlo/article/PIIS2214-109X(17)30070-0/fulltext"]The Lancet Global Health comment[/link]
