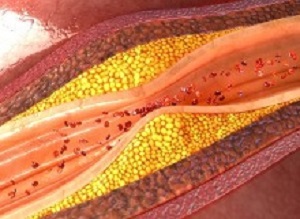
 Heart attacks are usually caused by inflamed plaques in the coronary artery causing an abrupt blockage of blood getting to the heart. The challenge for doctors is knowing which plaques are most likely to cause blockages, and therefore which patients should be treated with more aggressive therapies.
Heart attacks are usually caused by inflamed plaques in the coronary artery causing an abrupt blockage of blood getting to the heart. The challenge for doctors is knowing which plaques are most likely to cause blockages, and therefore which patients should be treated with more aggressive therapies.
The team at the University of Oxford has shown that the most dangerous plaques release chemical messengers which modify the surrounding fat. They have developed a technology that detects the inflamed plaques that are prone to cause heart attacks by analysing CT images of the fat surrounding the arteries.
Their new biomarker, called the Fat Attenuation Index (FAI), has been tested for the first time in a large study and was presented at the European Society of Cardiology Congress in Munich.
The study, supported by the British Heart Foundation and the NIHR Oxford Biomedical Research Centre, involved 3,900 patients from Europe (Erlangen, Germany) and the US (Cleveland Clinic), who were followed up for ten years after they had a CT coronary angiogram. The FAI technology was found to predict fatal heart attacks many years before they happen, with a significantly superior predictive accuracy compared with other methods. People with abnormal FAI had up to nine times higher risk of having a fatal heart attack in the next five years. Importantly, these patients would be the ideal candidates for aggressive medical therapy to prevent this from happening.
Every year, over 100,000 people die from a heart attack or related stroke in the UK alone, and heart disease and stroke remain the two biggest overall causes of death worldwide. Yet there is no method that allows for early detection of a potentially fatal build-up of plaque that could trigger a heart attack. With this new technology, clinicians would be able to identify those at risk of having a fatal heart attack in the next few years and take preventative steps before it strikes.
Professor Charalambos Antoniades, who led the study at the University of Oxford’s division of cardiovascular medicine, said: “This new technology may prove transformative for primary and secondary prevention. For the first time we have a set of biomarkers, derived from a routine test that is already used in everyday clinical practice, that measures what we call the ‘residual cardiovascular risk’, currently missed by all risk scores and non-invasive tests.
“Knowing who is at increased risk for a heart attack could allow us to intervene early enough to prevent it. I expect these biomarkers to become an essential part of standard CT coronary angiography reporting in the coming years.”
Professor Stephan Achenbach, from the University of Erlangen, said: “This study highlights an entirely new way in which patients at risk for myocardial infarction or heart attack could possibly be identified very early on. We very much need such novel approaches since a large part of all heart attacks occur without any prior notice. This study and its results may add to our armamentarium to prevent heart attacks, which makes the results so exciting from a scientific and clinical point of view.”
Professor Milind Desai, from Cleveland Clinic, said: “This is an exciting new technology which has the potential for providing a simple, non-invasive answer to detect patients at risk for future fatal heart attacks. More importantly, it highlights the incredible value of cross-continent collaboration to validate the findings in different populations.”
Professor Metin Avkiran, associate medical director at the British Heart Foundation, which funded the research, said: “Most heart scans are good at spotting blockages caused by large plaques, but not the smaller, high-risk plaques that are likely to rupture and cause a heart attack. This new technique could be a game changer – allowing doctors to spot those ‘ticking time bomb’ patients who are most at risk of a heart attack, and getting them on to intensive treatment. This would undoubtedly save lives.
“By using this non-invasive scan, we could prevent a lurking heart attack that might occur down the road. But it also potentially gives us a real-time window into tracking the effect of drugs on inflamed arteries, helping us to identify new life-saving therapies.”
The University of Oxford has formed a spinout company which has an exclusive licence to develop the FAI as a Software-as-a-Service offering, and which will be the vehicle that brings it to the healthcare sector to positively influence patient care. More details will follow shortly.
Summary
Background: Coronary artery inflammation inhibits adipogenesis in adjacent perivascular fat. A novel imaging biomarker—the perivascular fat attenuation index (FAI)—captures coronary inflammation by mapping spatial changes of perivascular fat attenuation on coronary computed tomography angiography (CTA). However, the ability of the perivascular FAI to predict clinical outcomes is unknown.
Methods: In the Cardiovascular RISk Prediction using Computed Tomography (CRISP-CT) study, we did a post-hoc analysis of outcome data gathered prospectively from two independent cohorts of consecutive patients undergoing coronary CTA in Erlangen, Germany (derivation cohort) and Cleveland, OH, USA (validation cohort). Perivascular fat attenuation mapping was done around the three major coronary arteries—the proximal right coronary artery, the left anterior descending artery, and the left circumflex artery. We assessed the prognostic value of perivascular fat attenuation mapping for all-cause and cardiac mortality in Cox regression models, adjusted for age, sex, cardiovascular risk factors, tube voltage, modified Duke coronary artery disease index, and number of coronary CTA-derived high-risk plaque features.
Findings: Between 2005 and 2009, 1872 participants in the derivation cohort underwent coronary CTA (median age 62 years [range 17–89]). Between 2008 and 2016, 2040 patients in the validation cohort had coronary CTA (median age 53 years [range 19–87]). Median follow-up was 72 months (range 51–109) in the derivation cohort and 54 months (range 4–105) in the validation cohort. In both cohorts, high perivascular FAI values around the proximal right coronary artery and left anterior descending artery (but not around the left circumflex artery) were predictive of all-cause and cardiac mortality and correlated strongly with each other. Therefore, the perivascular FAI measured around the right coronary artery was used as a representative biomarker of global coronary inflammation (for prediction of cardiac mortality, hazard ratio [HR] 2·15, 95% CI 1·33–3·48; p=0·0017 in the derivation cohort, and 2·06, 1·50–2·83; p<0·0001 in the validation cohort). The optimum cutoff for the perivascular FAI, above which there is a steep increase in cardiac mortality, was ascertained as −70·1 Hounsfield units (HU) or higher in the derivation cohort (HR 9·04, 95% CI 3·35–24·40; p<0·0001 for cardiac mortality; 2·55, 1·65–3·92; p<0·0001 for all-cause mortality). This cutoff was confirmed in the validation cohort (HR 5·62, 95% CI 2·90–10·88; p<0·0001 for cardiac mortality; 3·69, 2·26–6·02; p<0·0001 for all-cause mortality). Perivascular FAI improved risk discrimination in both cohorts, leading to significant reclassification for all-cause and cardiac mortality.
Interpretation: The perivascular FAI enhances cardiac risk prediction and restratification over and above current state-of-the-art assessment in coronary CTA by providing a quantitative measure of coronary inflammation. High perivascular FAI values (cutoff ≥–70·1 HU) are an indicator of increased cardiac mortality and, therefore, could guide early targeted primary prevention and intensive secondary prevention in patients.
Authors
Evangelos K Oikonomou, Mohamed Marwan, Milind Y Desai, Jennifer Mancio, Alaa Alashi, Erika Hutt Centeno, Sheena Thomas, Laura Herdman, Christos P Kotanidis, Katharine E Thomas, Brian P Griffin, Scott D Flamm, Alexios S Antonopoulos, Cheerag Shirodaria, Nikant Sabharwal, John Deanfield, Stefan Neubauer, Jemma C Hopewell, Keith M Channon, Stephan Achenbach, Charalambos Antoniades
[link url="http://www.ox.ac.uk/news/2018-08-28-study-shows-new-technology-can-predict-fatal-heart-attacks"]University of Oxford material[/link]
[link url="https://www.thelancet.com/journals/lancet/article/PIIS0140-6736(18)31114-0/fulltext"]The Lancet article summary[/link]
