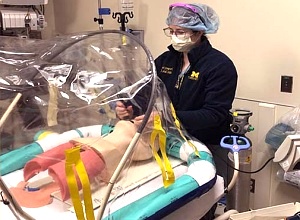
The International Union Against Tuberculosis and Lung Disease (The Union) has described the development of two novel devices, a negative pressure procedural tent and a portable helmet device, as having the potential to protect healthcare workers and transform the care of COVID-19 patients across the globe. The devices were developed by a team of engineering and medical staff at the University of Michigan and should be available by the end of 2020.
Both devices create a negative pressure environment for the wearer, which is essential for severely ill COVID-19 patients as a negative pressure environment prevents the infected air from a person with SARS-CoV-2, the organism causing COVID-19, from escaping into the wider environment. Hospitals typically treat such patients in a specially equipped negative pressure room.
“Clinical distancing is COVID-19’s next game-changer,” said Dr Paula I Fujiwara, Scientific Director of The Union. “There is no doubt that if both the portable helmet and tent are carried through to production and distributed by year’s end, we will see dramatic changes in the way in which severely ill patients with COVID-19 are treated, while at the same time providing vital protection for the healthcare workers caring for them.
“Both devices have the potential to be used widely in low- and middle-income countries, as well as in humanitarian settings where negative pressure rooms are just simply non-existent in so many locations. These devices could save countless preventable deaths from the COVID-19 virus but also other respiratory diseases such as tuberculosis. The Union salutes the fine work of the engineering and medical teams at the University of Michigan.
“The Union has long argued that innovation in research is key to responding to infectious diseases and we will proactively reach out to partner with organisations that can help us deliver on our promise of finding health solutions for those living in poverty by delivering new technologies for use in low- and middle-income settings where we have strong relationships, such as sub-Saharan Africa and India.”
The COVID-19 pandemic has put a severe strain on hospital environments and intensive care units (ICUs). Extensive efforts have been undertaken to provide adequate personal protective equipment (PPE) and isolation equipment (including the use of negative pressure rooms) to ensure patient and healthcare worker safety. However, many countries continue to have shortages of both, and some therapies for COVID-19 are associated with high rates of aerosolisation, which increases the safety threat faced by health care workers. Efforts to mitigate these risks are therefore paramount for the safety of patients and healthcare workers.
Patients with COVID-19 may require aerosol generating procedures (AGP) or therapies (including intubation, extubation, nebulised breathing treatments, non-invasive ventilation (NIV), heated high-flow nasal cannula (HHFNC), tracheostomy, and cardiopulmonary resuscitation. These factors amplify the risks faced by healthcare workers and are further magnified in low- and-middle-income countries, where access to safety equipment may be limited. Healthcare workers’ fear of contracting the virus could lead to deviations from standard care.
Strategies to mitigate these risks are certainly needed. “Clinical distancing,” a parallel to the practice of social distancing, has been proposed for healthcare workers to reduce unnecessary contact with patients to reduce transmission.
Currently, the negative pressure procedural tent and portable helmet device are being tested on site at the University of Michigan’s hospital by medical staff on consenting severely ill COVID-19 patients through an innovative care guideline. Manufacturing is planned for the end of the summer with the aim of having both devices available in hospitals by the end of 2020. The devices are also suitable for treating other respiratory diseases such as tuberculosis and influenza.
[link url="https://www.theunion.org/news-centre/news/rapid-development-of-equipment-covid-19?utm_source=Union+Global+Press+Contacts&utm_campaign=5658a6aeba-EMAIL_CAMPAIGN_2018_08_03_05_42_COPY_01&utm_medium=email&utm_term=0_b4b91f9ccc-5658a6aeba-518459853"]International Journal of Tuberculosis and Lung Disease material[/link]