 Doctors in the US have pioneered an anew treatment for spina bifida in which the baby is operated on before birth.
Doctors in the US have pioneered an anew treatment for spina bifida in which the baby is operated on before birth.
Spina bifida occurs when a baby’s spine and spinal cord do not develop properly causing a gap in the spine. It affects 24 babies in 100,000 and there are 14,000 people living with the condition in Britain which leaves sufferers unable to walk, with fluid build-up in the brain, lack of bladder control and other complications.
The report says foetal surgery for spina bifida has been common since the 1990s, but trying to repair the spine while the baby is still inside its mother is fraught with difficulty and cutting into the womb risks premature birth.
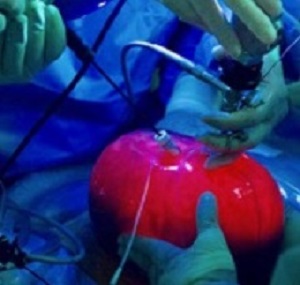
Now Dr Michael Belford, of Baylor College of Medicine, in Houston, Texas, has developed a new technique to remove the baby and womb so that spinal defect can be fixed before amniotic fluid eats away further at the gap in the spinal nerve tissue. Although the womb is still attached to the mother, once outside her body doctors can drain it, light it up and operate through tiny incisions.
The report says one of the first operations was performed last month on hairdresser Lexi Royer, 28, who was initially offered an abortion, but chose instead to take part in the experimental surgery when her baby was 24 weeks. “It sounded like we were looking at brain damage, feeding tubes, a breathing tube, a wheelchair, just a bad quality of life,” Royer is quoted as saying. “It’s not done by any means, but I definitely feel it’s the right thing for us. Seeing the ultrasound and how good he’s doing, moving his ankles and feet, it’s such a happy moment. I can’t imagine going on further in the pregnancy not knowing every day what damage is being done and if he’s getting worse. It’s such a relief to move forward.”
The report says during the three hour operation at Texas Children's Hospital in Houston, Belfort opened Royer’s abdomen but instead of cutting into the uterus, removed the whole womb through the hole. He then made two slits in the womb, one for a foetoscope – a tiny camera designed to light up and film inside – and another for surgical tools. Doctors pumped in carbon dioxide to keep the uterus buoyant, giving the, room to work and allowing them to see the spine more easily.
After injecting the foetus with anaesthetic, the team moved skin over the exposed spinal cord and stitched it in place. Doctors then refilled the womb with saltwater and replaced it back into Royer.
To develop the procedure, the report says Belfort and colleague Dr Whitehead spent two years practicing on sheep and a rubber ball with a doll insider wrapped in chicken skin to mimic the defect in spina bifida.
The team is now reporting on their work following 28 successful operations in which no foetuses have died, and only a few have needed shunts to drain fluid from the brain. Some of the mothers have also not needed caesarean sections.
The report says Belfort is now helping to train colleagues at Stanford University, however some doctors have warned that pumping the womb with carbon dioxide during the procedure could damage the baby, and cause neurological problems in later life.
Dr Katie Morris, senior clinical lecturer and consultant in maternal foetal medicine, University of Birmingham, said women in Britain would still be sent for in-utero surgery at present because there was more evidence needed to show the new technique was as safe.
“All of these techniques are exciting and novel in that they give an option for in-utero therapy but as the number of cases are small this is not something that will become widely available and at present if women come to our foetal medicine centre and request foetal surgery we refer to Belgium for open surgery as there are longer term outcomes available,” she said.
Abstract
Objective: To describe development of a two-port fetoscopic technique for spina bifida repair in the exteriorized, carbon dioxide-filled uterus and report early results of two cohorts of patients: the first 15 treated with an iterative technique and the latter 13 with a standardized technique.
Methods: This was a retrospective cohort study (2014-2016). All patients met Management of Myelomeningocele Study selection criteria. The intraoperative approach was iterative in the first 15 patients and was then standardized. Obstetric, maternal, fetal, and early neonatal outcomes were compared. Standard parametric and nonparametric tests were used as appropriate.
Results: Data for 28 patients (22 endoscopic only, four hybrid, two abandoned) are reported, but only those with a complete fetoscopic repair were analyzed (iterative technique [n=10] compared with standardized technique [n=12]). Maternal demographics and gestational age (median [range]) at fetal surgery (25.4 [22.9-25.9] compared with 24.8 [24-25.6] weeks) were similar, but delivery occurred at 35.9 (26-39) weeks of gestation with the iterative technique compared with 39 (35.9-40) weeks of gestation with the standardized technique (P<.01). Duration of surgery (267 [107-434] compared with 246 [206-333] minutes), complication rates, preterm prelabor rupture of membranes rates (4/12 [33%] compared with 1/10 [10%]), and vaginal delivery rates (5/12 [42%] compared with 6/10 [60%]) were not statistically different in the iterative and standardized techniques, respectively. In 6 of 12 (50%) compared with 1 of 10 (10%), respectively (P=.07), there was leakage of cerebrospinal fluid from the repair site at birth. Management of Myelomeningocele Study criteria for hydrocephalus-death at discharge were met in 9 of 12 (75%) and 3 of 10 (30%), respectively, and 7 of 12 (58%) compared with 2 of 10 (20%) have been treated for hydrocephalus to date. These latter differences were not statistically significant.
Conclusion: Fetoscopic open neural tube defect repair does not appear to increase maternal-fetal complications as compared with repair by hysterotomy, allows for vaginal delivery, and may reduce long-term maternal risks.
Authors
Belfort MA, Whitehead WE, Shamshirsaz AA, Bateni ZH, Olutoye OO, Olutoye OA, Mann DG, Espinoza J, Williams E, Lee TC, Keswani SG, Ayres N, Cassady CI, Mehollin-Ray AR, Sanz Cortes M, Carreras E, Peiro JL, Ruano R, Cass DL
[link url="http://www.telegraph.co.uk/science/2017/10/24/womb-view-surgeons-remove-uterus-mother-operate-spina-bifida/"]The Daily Telegraph report[/link]
[link url="https://www.ncbi.nlm.nih.gov/pubmed/28277363"]Obstetrics and Gynaecology abstract[/link]
