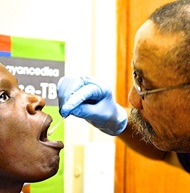
 Drawing inspiration from veterinary medicine, researchers at the University of Washington have helped developed a new prospective approach to detect tuberculosis (TB) – easy-to-obtain oral swab samples, greatly improving on standard diagnostics. "Care and control of the disease TB really requires prompt case-finding," said Gerald Cangelosi, UW professor of environmental and occupational health sciences and global health. Detecting the disease with a simple oral swab "could be a game changer for TB control because it could make diagnosis cheaper and easier," he said.
Drawing inspiration from veterinary medicine, researchers at the University of Washington have helped developed a new prospective approach to detect tuberculosis (TB) – easy-to-obtain oral swab samples, greatly improving on standard diagnostics. "Care and control of the disease TB really requires prompt case-finding," said Gerald Cangelosi, UW professor of environmental and occupational health sciences and global health. Detecting the disease with a simple oral swab "could be a game changer for TB control because it could make diagnosis cheaper and easier," he said.
Cangelosi is corresponding author on a paper detailing the new acquisition method, discovered with researchers at the South African Tuberculosis Vaccine Initiative and the University of Cape Town, South Africa led by Dr Angelique Luabeya.
Diagnosing TB conventionally involves collecting and testing a person's sputum – thick, gluey mucus coughed up from the lungs. Working with sputum samples is challenging due to the material's "horribly gloppy" nature, as Cangelosi described it. Sputum can hide pathogens from pathologists because it is difficult to dislodge bacteria from within the mucus' milieu. Also, in order to produce sputum, patients must cough, which puts sample-collecting public health workers at risk for contracting the disease.
In search of a viable alternative to sputum samples, the scientists swabbed the mouths of 20 healthy individuals and 20 TB patients. Samples from patients with confirmed TB were collected in a clinic in South Africa. The control samples were taken from healthy individuals in Washington state. Lisa Jones-Engel, a research scientist with the UW National Primate Research Centre, advised the study team as they applied the oral swab method to human disease. Rachel Wood, at UW's Department of Environmental and Occupational Health Sciences and other researchers detected TB in oral swabs taken from 18 of the 20 confirmed patients. None of the samples from healthy volunteers tested positive.
Previous efforts to test for TB in materials other than sputum, such as blood, urine or exhaled breath, have been limited by much lower accuracy, with detection rates typically below 50%. Moreover, safely obtaining blood or urine samples requires specialised certification, whereas volunteers with minimal training may collect oral swabs. This could open the door to widespread implementation of this new approach.
A long-term goal is to enable active TB case finding, in which at-risk populations are screened for the disease to identify and prevent opportunities for transmission. Cangelosi stressed that the study is merely a proof of principle, limited by its small size. Efforts are under way to expand this initial study into a large-scale controlled trial. Yet the preliminary success offers hope for greatly improved TB detection and control, especially in nations with limited public health resources.
[link url="http://hsnewsbeat.uw.edu/story/simple-swab-test-holds-promise-ease-tuberculosis-detection"]University of Washington material[/link]
[link url="http://www.nature.com/srep/2015/150302/srep08668/full/srep08668.html"]Scientific Reports abstract[/link]
