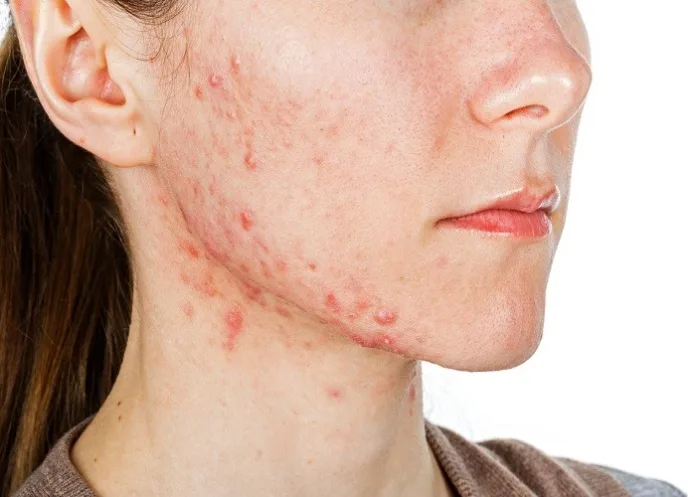
A cheap drug used to treat high blood pressure could help thousands of women suffering from persistent acne, according to a study led by the University of Southampton and involving more than 400 women.
After 12 weeks, said the researchers, those taking spironolactone – which works by reducing the main hormone leading to the development of acne – saw a huge improvement, reports BBC News.
“Compared with those on the placebo, the women on spironolactone saw a significant improvement in their acne after 12 and 24,” said Professor Miriam Santer, GP and co-lead of the trial.
She said spironolactone could offer an alternative to antibiotics for many women with persistent acne, to use alongside topical acne treatments.
Acne vulgaris is very common in adolescence and often persists into adulthood often causing substantial social and psychological effects on the sufferers.
UK guidance recommends fixed combination topical preparations containing retinoids, benzoyl peroxide or antibiotics as a first line treatment for mild to moderate acne or, for moderate to severe acne, a fixed combination topical agent alone or with oral lymecycline or doxycycline.
National Institute for Health and Care Excellence’s guidance recommends that treatment regimens which include an antibiotic (topical or oral) should not be continued for more than six months unless in exceptional circumstances (other guidelines limit oral antibiotic duration to three months).
However, doctors report barriers to discontinuing oral antibiotics once they have been started.
A third of people with acne receive long courses of oral antibiotics (28 days or more), with acne accounting for most antibiotic exposure among people of 11-21 in England.
But increasing prevalence of antibiotic resistance mean alternatives to antibiotics are urgently needed, which is where the researchers believe spironolactone could play a role.
Spironolactone is a potassium-sparing diuretic widely used for indications such as hypertension, and has been prescribed off-licence for acne for many years because of its anti-androgenic properties.
However, systematic reviews have highlighted a paucity of evidence from randomised controlled trials, with the largest trial to date including only 34 participants.
The latest Spironolactone for Adult Female Acne (SAFA) trial aimed to evaluate whether spironolactone improves acne in women with persistent facial acne compared with placebo, in addition to use of standard topical care.
The scientists’ findings present an affordable, antibiotic-free alternative for acne sufferers.
One of the trial participants said she had suffered from severe acne since her teens and used numerous prescribed creams and antibiotics, as well as the contraceptive pill to try to control it, without success.
Within three months of starting on the spironolactone for adult female acne (SAFA) trial at Poole Hospital, “everything was gone, all the spots had disappeared”.
Since the trial, she has stayed on spironolactone and has been acne-free for more than two years.
The study was published in The British Medical Journal (BMJ).
Study details
Effectiveness of spironolactone for women with acne vulgaris (SAFA) in England and Wales: pragmatic, multicentre, phase 3, double blind, randomised controlled trial
Miriam Santer, Megan Lawrence, Alison Layton, et al.
Published in The BMJ on 16 May 2023
Abstract
Objective
To assess the effectiveness of oral spironolactone for acne vulgaris in adult women.
Design
Pragmatic, multicentre, phase 3, double blind, randomised controlled trial.
Setting
Primary and secondary healthcare, and advertising in the community and on social media in England and Wales.
Participants
Women (≥18 years) with facial acne for at least six months, judged to warrant oral antibiotics.
Interventions
Participants were randomly assigned (1:1) to either 50 mg/day spironolactone or matched placebo until week six, increasing to 100 mg/day spironolactone or placebo until week 24. Participants could continue using topical treatment.
Main outcome measures
Primary outcome was Acne-Specific Quality of Life (Acne-QoL) symptom subscale score at week 12 (range 0-30, where higher scores reflect improved QoL). Secondary outcomes were Acne-QoL at week 24, participant self-assessed improvement; investigator’s global assessment (IGA) for treatment success; and adverse reactions.
Results
From 5 June 2019 to 31 August 2021, 1267 women were assessed for eligibility, 410 were randomly assigned to the intervention (n=201) or control group (n=209) and 342 were included in the primary analysis (n=176 in the intervention group and n=166 in the control group). Baseline mean age was 29.2 years (standard deviation 7.2), 28 (7%) of 389 were from ethnicities other than white, with 46% mild, 40% moderate, and 13% severe acne. Mean Acne-QoL symptom scores at baseline were 13.2 (standard deviation 4.9) and at week 12 were 19.2 (6.1) for spironolactone and 12.9 (4.5) and 17.8 (5.6) for placebo (difference favouring spironolactone 1.27 (95% confidence interval 0.07 to 2.46), adjusted for baseline variables). Scores at week 24 were 21.2 (5.9) for spironolactone and 17.4 (5.8) for placebo (difference 3.45 (95% confidence interval 2.16 to 4.75), adjusted). More participants in the spironolactone group reported acne improvement than in the placebo group: no significant difference was reported at week 12 (72% v 68%, odds ratio 1.16 (95% confidence interval 0.70 to 1.91)) but significant difference was noted at week 24 (82% v 63%, 2.72 (1.50 to 4.93)). Treatment success (IGA classified) at week 12 was 31 (19%) of 168 given spironolactone and nine (6%) of 160 given placebo (5.18 (2.18 to 12.28)). Adverse reactions were slightly more common in the spironolactone group with more headaches reported (20% v 12%; p=0.02). No serious adverse reactions were reported.
Conclusions
Spironolactone improved outcomes compared with placebo, with greater differences at week 24 than week 12. Spironolactone is a useful alternative to oral antibiotics for women with acne.
BBC News article – Cheap blood pressure drug could treat acne, Southampton study finds (Open access)
See more from MedicalBrief archive
Call for tighter safety measures for acne drug linked to suicides
Diuretic drug found to be successful in treatment of acne
How skin oil turns infection-fighting cells into accomplices, making acne bacteria thrive – US study
Doctors now favouring combination therapies to treat acne