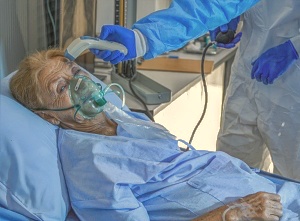
A small but significant number of people are suffering from the “long tail” form of the virus, with “constantly shifting and bizarre symptoms”, writes Paul Garner, professor of infectious diseases at the Liverpool School of Tropical Medicine, in the BMJ.
In mid-March Paul Garner developed what he thought was a “bit of a cough”. A professor of infectious diseases, Garner was discussing the new coronavirus with David Nabarro, the UK’s special envoy on the pandemic. At the end of the Zoom call, Nabarro advised Garner to go home immediately and to self-isolate. Garner did. He felt no more than a “little bit off”.
The Guardian reports that days later, he found himself fighting a raging infection. It’s one he likens to being “abused by somebody” or clubbed over the head with a cricket bat. “The symptoms were weird as hell,” he says. They included loss of smell, heaviness, malaise, tight chest and racing heart. At one point Garner thought he was about to die. He tried to Google “fulminating myocarditis” but was too unwell to navigate the screen.
Garner refers to himself wryly as a member of the “Boris Johnson herd immunity group”. This is the cluster of patients who contracted COVID-19 in the 12 days before the UK finally locked down. He assumed his illness would swiftly pass. Instead it went on and on – a rollercoaster of ill health, extreme emotions and utter exhaustion, he said in a blog post.
There is growing evidence that the virus causes a far greater array of symptoms than was previously understood. And that its effects can be agonisingly prolonged: in Garner’s case for more than seven weeks. The professor at the Liverpool School of Tropical Medicine says his experience of COVID-19 featured a new and disturbing symptom every day, akin to an “advent calendar”.
He had a muggy head, upset stomach, tinnitus, pins and needles, breathlessness, dizziness and arthritis in the hands. Each time Garner thought he was getting better the illness roared back. It was a sort of virus snakes and ladders. “It’s deeply frustrating. A lot of people start doubting themselves,” he says. “Their partners wonder if there is something psychologically wrong with them.”
Since his piece was published, Garner has received emails and tearful phone calls from grateful readers who thought they were going mad. “I’m a public health person,” he says. “The virus is certainly causing lots of immunological changes in the body, lots of strange pathology that we don’t yet understand. This is a novel disease. And an outrageous one. The textbooks haven’t been written.”
Professor Tim Spector, of King’s College London, estimates that a small but significant number of people are suffering from the “long tail” form of the virus. Spector is head of the research group at King’s College London which has developed the COVID-19 tracker app. This allows anyone who suspects they have the disease to input their symptoms daily; some 3m to 4m people are currently using it, mostly Britons and Americans.
Spector estimates that about 200,000 of them are reporting symptoms which have lasted for the duration of the study, which is six weeks. There is good clinical data available for patients who end up in hospital.
“These people may be going back to work and not performing at the top of their game,” Spector says. “There is a whole other side to the virus which has not had attention because of the idea that ‘if you are not dead you are fine.’
The Guardian reports that scientific explanations for what is happening are still at an early stage. Lynne Turner-Stokes, professor of rehabilitation medicine at King’s College, says COVID is a “multi-system disease” which can potentially affect any organ. It causes microvascular problems and clots. Lungs, brain, skin, kidneys and the nervous system may be affected. Neurological symptoms can be mild (headache) or severe (confusion, delirium, coma).
Turner-Stokes says it’s uncertain why the illness is sometimes so protracted. Researchers are now collaborating across borders. They are examining the latest data from European countries ahead of the UK in pandemic terms, such as Italy and Spain, as well as China. They are seeking to work out what support may be needed for severe and chronic patients, with COVID posing similar challenges to HIV/Aids a generation ago.
[link url="https://www.theguardian.com/world/2020/may/15/weird-hell-professor-advent-calendar-covid-19-symptoms-paul-garner?CMP=Share_iOSApp_Other"]Full report in The Guardian[/link]
[link url="https://blogs.bmj.com/bmj/2020/05/05/paul-garner-people-who-have-a-more-protracted-illness-need-help-to-understand-and-cope-with-the-constantly-shifting-bizarre-symptoms/"]BMJ blog[/link]