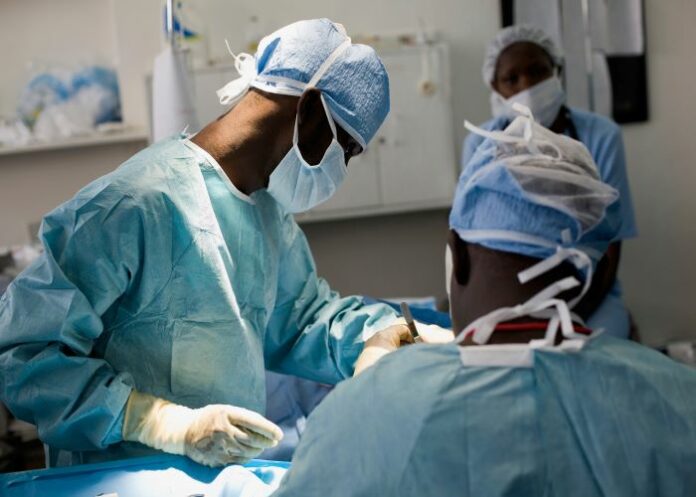
National Department of Health statistics reveal that more than 107,000 non-emergency or elective surgeries were put on the back burner during the COVID-19 pandemic. But challenges in addressing surgical backlogs were there long before COVID-19, writes Alicestine October for Spotlight.
Professor Kathryn Chu, director of the Centre for Global Surgery at Stellenbosch University’s Faculty of Medicine and Health Sciences, said compared with infectious diseases like HIV, TB, and COVID-19, surgical conditions and care were not a major priority in the public health system.
“Surgery as a whole has not really had a national strategy or plan and that is a problem,” she said. “Our government and province do not have a co-ordinated surgical plan. There’s nothing in the National Health Plan about surgery – it’s not even mentioned.”
The makings of a plan but no funding
Chu said in 2019, a Technical Working Group on National Safe Surgical Care was formed to write a national surgical plan. This is now an official Ministerial Advisory Committee, Chu being a member of the core team. “And now that NHI is coming, the idea is to have a surgical benefits package defined through this and there will be different factors to consider to identify surgical best buys, which conditions should be covered, how much should it cost the system – the burden of disease of that surgical condition, etcetera.”
The plan – a National Surgical Obstetric and Anaesthesia Plan (NSOAP) for South Africa – is described as a “blueprint to define a national surgical package of care” and focuses on key areas including human resources, service delivery, infrastructure, supply chain, governance, finance and informatics. Among the main objectives are ensuring the “implementation of an equitable, accessible and comprehensive surgical, obstetric and anaesthesia care system” for SA.
The plan’s initial start date for implementation was January 2022. But according to Chu, there have been many delays and the research is still under way. She says there are quite a lot of challenges and no money forthcoming from government to fund this.
“It’s still planned but there are definitely delays. It is still very necessary but is taking longer than we thought. It’s going to cost millions of rands to even do the work. Government will have to put in the money if they want to prioritise this.”
Spotlight asked health spokesperson Foster Mohale about the progress and resources but had not received a response by the time of publication.
Shortages in the surgical workforce and the maldistribution of surgical capacity have been a particular challenge over the years, said Chu. Many specialists are in the private sector and those in the public sector are often working in the bigger tertiary hospitals in urban centres.
For 12 to 18 months almost no elective surgeries were done during COVID. At present, all hospitals have different strategies to deal with surgical backlogs and some direction from the provinces or national government could be helpful.
For instance, COVID-19, fire, theft and infrastructural damage, among other things, have had such dire consequences at Charlotte Maxeke Johannesburg Academic Hospital that children can wait between six months and two years for surgery in some cases, said Gauteng Health MEC Nomathemba Mokgethi.
Responding to a question in the provincial legislature, she said the longest waiting list was for orthopaedics, with 833 patients who might wait up to two years for surgery, reports TimesLIVE.
In 2021, 785 operations were cancelled at the hospital, adding to the 2,677-strong patient waiting list.
Mokgethi said 453 paediatric patients will wait for surgery and 610 patients had cancelled operations. The other cancellations were:
• 80 cardiothoracic operations;
• 40 gastrointestinal operations;
• 25 breast clinic, endocrine and soft-tissue operations;
• 20 neurosurgery operations; and
• 10 ear, nose and throat operations.
Some 200 cataract patients have a delay of between six and eight months for surgery, 137 neurosurgery patients will wait for six months, and 109 urology (urinary-tract system) patients will wait between four and six months.
Mokgethi was responding to DA Gauteng shadow health MEC MPL Jack Bloom, who said these numbers “underestimate the true situation, as they leave out the long waiting periods for many patients to be diagnosed by a specialist before they are placed on the waiting lists for surgery”.
Exploring solutions
1. Devolving surgical care
One way to better co-ordinate surgical care would be to devolve some procedures to smaller district hospitals closer to patients.
Chu, however, said district hospitals are hamstrung by resource and capacity constraints. Many do not have the necessary ICUs and CT scanners, and various equipment for post-operative care are unavailable. So the surgical care package they can provide is limited, she said.
“Regional hospitals do what we call ‘bread and butter’ surgery: most have some good capacity but there are many district hospitals that are smaller and in rural areas that should (based on international practice) provide basic surgical care. But what that surgical package of care should look like is not well defined – specifically in South Africa.”
On possible solutions to improve the co-ordination of surgical care, Associate Professor Lydia Cairncross, University of Cape Town Global Surgery Oncology Lead at Groote Schuur Hospital, said from a cost-efficiency point of view it was much better to treat patients at a district rather than central hospital level.
“But lots of relatively minor surgery that could be done at district level hospitals is being done at central or regional hospitals,” said Cairncross. This adds to the service pressures at these hospitals. “So we must focus on the district hospitals and ensure they have the capacity to provide a package of surgical procedures.”
2. Beefing up the surgical workforce
Both Chu and Cairncross flagged staff shortages, especially of theatre nurses, as a huge challenge. Cairncross said an immediate priority for government is to unfreeze all posts so surgical teams can be capacitated. “I don’t know how to emphasise this enough,” she said. “There’s doublespeak happening where we talk about needing capacity, and human resources, but at the same time, we actually have a growing unemployment crisis among junior doctors. So there are people who can do the work but the funded posts are not available.”
National Health Department stats show that by May this year, there was a 15.47% vacancy rate of critical skills personnel in the nursing category, meaning 22 655 vacancies.
“When someone resigns or retires, the post is often left unfilled for six to 12 months and the whole system spirals into chaos. This obviously has knock-on effects with other people who then get burnt out and also leave,” said Cairncross. “So the first step in a national co-ordinated response would be to fill all theatre-related vacant posts as a matter of urgency.”
Chu echoed this, adding there was a shortage of nurses, with many of them already working maximum time shifts, so even opening up theatres on weekends would not really tackle all backlogs.
So far, the Health Department has been citing budget constraints for not filling posts in the public health sector immediately. Many health budgets, also in the Western Cape, took a knock with COVID-19. Chu said in the Western Cape, the government put money into a recovery plan. “But that was once-off and mostly, they want you to do more without necessarily increasing the resources.”
Again referring to district hospitals, she said these hospitals often have theatres that are empty most days because they don’t have the staff to run them, whereas tertiary hospitals – due to various surgical specialities – are almost always full. “So, if you’re looking for more theatres, one solution is to go to the smaller hospitals but surgeons need theatre nurses. We need to train more theatre nurses. One way to do this would be to have spent the money of the COVID surgical recovery on training more nurses but the province was thinking more of a quick fix.”
But Cairncross says there is a tremendous amount of red tape and bureaucracy around getting specialist nurses trained. “So, it doesn’t really help to train up GPs, which we can do. But to do these operations, you need a theatre team and the core of that team is the nursing team. We absolutely need to invest in training theatre nurses.”
What makes South Africa unique, Chu said, is you don’t have to be a specialist to perform surgery or anaesthesia. “There are many GPs and medical officers doing some operations and who give anaesthesia who never qualified as a specialist per se. But, their training is variable and not that well-regulated and there isn’t really a standard of care on what procedures they should know how to do. So it’s a bit hit or miss and personalised depending on where the person is working and who their mentor is,” she said.
Cairncross said SA needs a national plan for developing the human resources for surgery. “Not only the theatre team but also build that into the nursing teams in the ward and the post-operative rehabilitation, which includes physiotherapy, occupational therapy (OT). This all needs to be part of this planning.
“For example, you can do a really beautiful hand operation but if you don’t have physio and OT post-operatively it’s almost as though you didn’t do it. Your rehabilitation is a critical step in surgical care, which we can’t forget.”
Health Minister Dr Joe Phaahla recently said the South African Nursing Council’s figures showed 52,887 specialist nurses had completed their studies and registered as nursing specialists over the past decade. The figures, however, show that despite this, the number of appointments in the public sector remains low. This, among others, said Phaahla, was due to the private sector absorbing some nurse specialists such as ICU-trained nurses “prefer to work for agencies as proven during the height of the COVID-19 pandemic”.
3. Co-opting private sector resources
Another way to boost surgical capacity is to lean on the private sector. During COVID-19 there was a small taster of this when the government bought private sector beds for COVID-19 patients and paid specific amounts of money daily per patient.
But there are some considerations to remember.
Cairncross told Spotlight there were many levels at which there could be support between the two systems, for example, with theatre space. This would mean private hospital theatres being used for public sector patients. “The question then arises – who’s the theatre team that does that?” she said. “Is that the theatre team in the private hospital or are they coming from the public hospital? It’s a good solution on paper but in terms of hundreds of operations, it can be quite difficult.”
She said there were already some public/private programmes running, like some Saturday (surgery) lists being done in private hospitals. That helps, and should be encouraged, she added. “But the true impact comes from investing in building capacity in the public sector. So if you compare a once in a while Saturday list, maybe once a month or every two months in a private hospital to what we are trying to do and are doing without recovery, which is eight lists a week – it’s incomparable.”
Cairncross said another way the private sector could help was through sharing surgical expertise, especially in smaller district hospitals where there is a theatre and nursing staff but no anaesthetist or surgical expertise. “These skills can then be volunteered or contracted in or paid locum fees to support lists in those smaller hospitals,” she says, “but you still need a surgeon in the public sector screening and ensuring it’s the correct operation etc.”
TimesLIVE article – Long waiting times for child ops at Charlotte Maxeke Hospital (Open access)
See more from MedicalBrief archives:
Surgery catch-up stymied by South Africa’s shortage of ICU nurses
Retirement boom and training drought — SA’s looming nursing crisis
Tygerberg Hospital plea for more specialised nurses
Massive UK nursing shortage sucks in Kenyan, South African and Zimbabwean nurses
SA hospital groups pinched as elective surgeries end and occupancies plummet