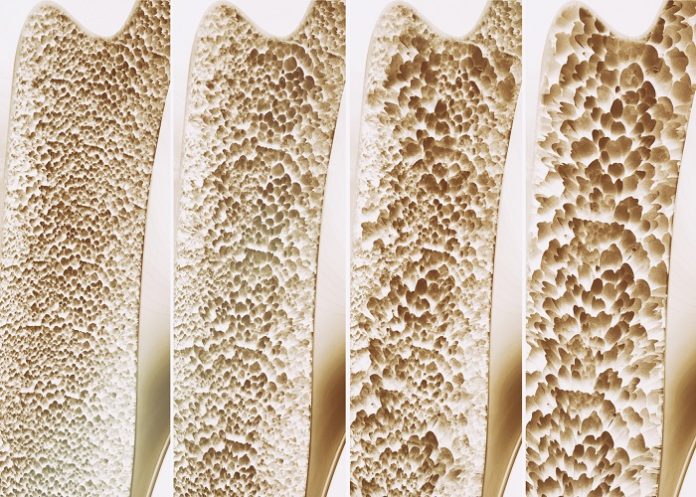
A large analysis has suggested that popular weight loss drugs may carry an increased risk to bone health, and conditions like osteoporosis, reports NBC News – while a second study, presented at the same event, suggested that women who start hormone replacement therapy (HRT) within a year after menopause may slash their risk of developing osteoporosis.
According to research presented last week at the American Academy of Orthopaedic Surgeons’ (AAOS) annual meeting in New Orleans recently, GLP-1 drugs, including Ozempic and Wegovy, could increase a woman’s chances of landing up with osteoporosis and/or gout.
Dr John Horneff, an associate Professor of Orthopaedic Surgery at the University of Pennsylvania and lead author of the study, said he began looking into the issue after some patients appeared to develop serious tendon tears after relatively minor injuries. That led them to examine whether GLP-1s might affect bone and other connective tissue more broadly.
“People are taking these medications, and obviously there’s a tremendous amount of upside,” Horneff said. “But with that, they start to decrease their intake of food and nutrients.”
Osteoporosis, which weakens the bones and makes them likelier to break or fracture, often from minor falls, is a common concern for many older adults and for people who lose a significant amount of weight quite quickly.
Gout, meanwhile, is a painful form of arthritis that can occur when the body has too much uric acid, which can come from a diet high in red meat and alcohol – as well as rapid weight loss.
In this latest study, which has not yet been published in a peer-reviewed journal, researchers analysed five years of medical records from more than 146 000 adults with a diagnosis of both obesity and type 2 diabetes.
The study compared patients taking GLP-1 drugs to patients not taking them.
The records didn’t include detailed information about which GLP-1 drug each patient was taking, though medications documented included semaglutide, sold as Ozempic and Wegovy, and liraglutide, sold as Victoza and Saxenda.
About 4% of GLP-1 users developed osteoporosis, compared with slightly more than 3% of non-users – an increased risk of about 30%. A related condition, osteomalacia, which involves the softening of the bones, was rare but also occurred about twice as often among people on GLP-1s.
Rates of gout were also slightly higher – 7.4% for GLP-1 users versus 6.6% for non-users – an increased risk about 12%.
“It’s not huge,” Horneff said. “But within that data that were put in there, you even saw nearly a doubling of the risk of having some sort of bone mineral density issue at five years.”
“Weight loss does cause bone loss,” said Dr Clifford Rosen, a Professor of Medicine at Tufts University who has been studying the potential impact of GLP-1s on bone health. He wasn’t involved with the new research.
“The question we’ve been studying is whether this is a normal compensation of the skeleton, it’s just reshaping itself, or whether this is truly a risk for losing bone that’s more rapid than what would be expected,” he added.
Because the new research was observational, it can’t prove the medications caused either condition. Horneff said the team didn’t know about patients’ diet or exercise habits, or whether they were taking vitamin D supplements or other nutrients important for bone health.
But the results echo other research, including a study published in February in the Journal of Clinical Endocrinology & Metabolism that linked GLP-1 drugs to a higher risk of osteoporosis-related fractures in older adults with type 2 diabetes.
The FDA notes in its label for semaglutide that it might increase the risk of bone fractures in older adults and women, Rosen said.
Dr Susan Spratt, an endocrinologist and the senior medical director for the Population Health Management Office at Duke Health in North Carolina, questioned whether the increased risk was due to the rapid weight loss or some other mechanism of the drug.
She said some studies have suggested musculoskeletal benefits with GLP-1 drugs and that she often sees improvements in joint pain among patients who lose weight on the medications. But she emphasised that joint health and bone density are not the same.
Horneff said more research is needed to understand why GLP-1 drugs might affect bone health.
One theory, he said, is that because the medications suppress appetite, some patients may not get enough key nutrients, like vitamin D and calcium, which are important for maintaining bone health.
Another possibility is that the rapid weight loss itself changes how the body builds and breaks down bone.
“It’s the same idea as when we always hear about astronauts going up into space and they’re in a gravity-zero environment for too long,” Horneff said.
“There’s nothing forcing their bones to kind of hold their weight anymore. And a lot of them come back with low bone density. So the thought is, these patients, their skeleton was used to kind of maintaining one frame, and then all of a sudden, that’s being decreased.”
For gout, Horneff said, rapid weight loss can lead to a temporary spike in uric acid, increasing the risk of gout.
Dr Christopher McGowan, a gastroenterologist who runs a weight loss clinic in Cary, North Carolina, said that even if GLP-1 drugs do increase the risk, it doesn’t mean patients are powerless. Other data, he said, suggest that when GLP-1s are combined with structured exercise, bone density loss is largely mitigated.
“That tells us lifestyle factors play a major role,” he said.
The research, McGowan said, shouldn’t alter the prescribing of GLP-1 medications. He said it’s a reminder that obesity treatment also requires guidance on protein intake, exercise and bone health monitoring.
“The takeaway isn’t fear. It’s refinement,” he said
Early HRT may cut osteoporosis risk
Meanwhile, at the same event, research presented by scientists from Stony Brook University, New York, suggested that women who start hormone-replacement therapy (HRT) within a year after menopause may have a lower risk of developing osteoporosis, reports Medscape.
The team used the health records database TriNetX to analyse data from more than 137 000 postmenopausal women under 60. They compared women who started HRT within a year of a menopause diagnosis to matched peers who did not receive HRT.
“The early HRT group was defined as those women receiving HRT within the first year of diagnosis of menopause,” said study author James Barsi, MD, an orthopaedic surgeon at Stony Brook Children’s Hospital in New York.
At three years, researchers found no statistically significant difference in osteoporosis diagnoses between the early HRT and no-HRT groups (1.11% vs 1.15%; risk ratio [RR] 1.03; 95% CI, 0.95-1.13; P = .449).
Within five years, however, women who did not receive HRT had a significantly higher rate of osteoporosis (2.08% vs 1.91%; RR, 1.09; 95% CI, 1.02-1.16; P = .010). At the final follow-up at five years, the gap widened further: 5.31% of women in the no-HRT group were diagnosed with osteoporosis compared with 4.39% in the early HRT group (RR 1.21; 95% CI, 1.16-1.26; P < .001).
Fracture outcomes followed a similar pattern. At three years, fracture rates did not significantly differ (1.94% vs 2.03%; RR, 1.05; 95% CI, 0.98-1.12; P = .171). By five years, fractures were modestly but significantly more common in women who did not receive HRT (3.55% vs 3.37%; RR, 1.05; 95% CI, 1.00-1.11; P = .034).
Cumulative fracture rates were 7.06% in the no-HRT group compared with 6.21% in the early HRT group (RR, 1.14; 95% CI, 1.10-1.18; P < .001).
While short-term fracture risk did not differ, the longer-term findings suggest cumulative skeletal benefits, Barsi said.
“Although we did not find a significant difference in fractures in the short term of three years, we did find differences in the medium to longer term,” said Barsi. “This would suggest that the effects of HRT seem to be more cumulative in nature and are protective in the long term.”
The study did not differentiate between oestrogen-only vs combined oestrogen-progestin therapy or whether the women took the therapies orally or transdermally.
“Unfortunately, the database did not get into the details of the type or route of hormone therapy received,” Barsi said.
According to Abigail Campbell, MD, a sports medicine orthopaedist and co-director of the Women’s Sports Medicine Centre at NYU Langone Health, New York City, the biological mechanism behind the findings is plausible, but she urged caution in interpretation.
“The reason women over 50 get osteoporosis is because their oestrogen level drops, which is protective against bone loss,” said Campbell, who was not involved in the study. “Hormone replacement gives back some of the oestrogen, so bone loss slows down.”
Campbell said the delayed separation in outcomes – with differences emerging at five years but not at three years – is consistent with how menopause unfolds.
However, she warned that increased public attention on hormone therapy may lead some patients to seek treatment inappropriately.
“Yes, it can do amazing things for the right person, but the problem with HRT is it’s not recommended or safe for everyone,” she said.
Some women, including those with a history of hormone-sensitive cancers, should not take hormone therapy, and their decisions should involve gynaecologists or menopause specialists, Campbell added.
For now, she suggested clinicians should continue recommending proven strategies for bone health.
“Weight-bearing exercise and resistance exercise have all been shown unequivocally to be important for bone health,” she said. “These are things we know are tried and true.”
See more from MedicalBrief archives:
Weight-loss drugs race now enters new phase
Why I think weight loss drugs are not the answer – US obesity expert
Why osteoporosis isn’t just a woman’s problem
NHS rolls out osteoporosis drug for menopausal women
Education needed regarding efficacy of HRT for most women
FDA plan to change ‘black box’ warning on HRT sparks concern