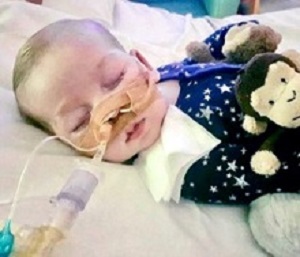
 Charlie Gard, the incurably ill British infant who died recently, could not hear, see or even cry. But, reports The New York Times, his case captured the attention of the pope and the US president, and raised difficult ethical issues that reverberated around the world.
Charlie Gard, the incurably ill British infant who died recently, could not hear, see or even cry. But, reports The New York Times, his case captured the attention of the pope and the US president, and raised difficult ethical issues that reverberated around the world.
He died with his parents by his side a day after the British High Court ruled that he could be moved to a hospice and that his life support could be withdrawn. In an emotional statement before the court, Charlie’s mother, Connie Yates, noted that her son had “had a greater impact on and touched more people in this world in his 11 months than many people do in a lifetime.”
The report says the infant had a rare and debilitating genetic condition known as mitochondrial DNA depletion syndrome. Charlie, who would have turned a year old on 4 August, was not able to peer at his parents’ faces. He also could not swallow.
The child’s final moments were not as his parents had hoped. The report says they fought a long and often tense battle in court to control his fate, to take him to the US for experimental treatment and, finally, to move him to their home in West London to die.
They lost their fight. Yates, who works as a caregiver, said in statement that the hospital had “denied us our final wish.” “Most people won’t ever have to go through what we have been through,” she said. “We’ve had no control over our son’s life and no control over our son’s death.”
But, the report says, the doctors treating Charlie at Great Ormond Street Hospital in central London countered that the “risk of an unplanned and chaotic end to Charlie’s life” at home was “unthinkable.” For months, the hospital had argued that he had irreversible brain damage, that the life support should be removed and that he should be allowed the right to die with dignity.
“We deeply regret that profound and heartfelt differences between Charlie’s doctors and his parents have played out in court over such a protracted period,” the hospital said. “We will never do anything that could cause our patients unnecessary and prolonged suffering.”
The report says the case laid bare several issues, among them: Should parents or doctors or the courts have the final say in irreconcilable disputes over the treatment of sick children? And at what point should the limits of medicine be recognised and the parents of an infant be compelled to let go?
Biomedical ethicists said the case offered a cautionary tale of how a legal battle, scrutiny by the global news media and intractable differences between parents and doctors can spiral out of control in the social media age. Both the hospital and the parents in the Gard case dug in, their arguments playing out on Facebook and Twitter and capturing the attention of world figures including President Trump and Pope Francis.
Dr Robert D Truog, a physician at the pediatric intensive-care unit at Boston Children’s Hospital and the director of the Centre for Bioethics at Harvard Medical School, said in the report that “Charlie’s parents were like parents all over the world – they were willing to do absolutely anything to save the life of their child.” He added: “They were the victims, not the cause, of this tragic situation.”
The report says parents’ raw emotions played out in the courtroom, where Yates broke down in tears of frustration, at one point shouting, “What if it was your child?” before fleeing the room. At another moment, Gard, a mailroom worker, cried out, “Evil” after a hospital lawyer spoke. On several occasions, both parents stormed out of the courtroom. Some of the lawyers and journalists covering the case were reduced to tears.
The report says the case went through several courts, including the UK Supreme Court and the European Court of Human Rights, which backed the hospital’s views, in part because experts said Charlie could be suffering. His parents insisted he was not.
In most cases, medical experts say, doctors decide when to remove life support from an incurably ill child, in consultation with parents, and these cases rarely wind up in court. But in Britain, the courts are the final arbiter when irreconcilable disputes arise.
The report says the case also spurred questions about the wisdom of offering parents the hope of experimental treatment when faced with an incurable disease. That debate took center stage after Dr Michio Hirano, a neurologist at Columbia University Medical Centre in New York, offered Charlie’s parents a ray of hope that an experimental treatment known as nucleoside therapy could improve Charlie’s condition.
The treatment had been tested on mice and on 18 people with a mutation in a gene known as TK2. But it had never been tried on someone with Charlie’s particularly debilitating form of mitochondrial DNA depletion syndrome, which is caused by a different genetic mutation.
During an often-acrimonious and emotional High Court hearing this month, Charlie’s parents argued that he should be allowed to receive the experimental treatment. But lawyers for Great Ormond Street Hospital countered that Hirano had held out hope without even examining the child or reviewing his full medical charts.
(Hirano said in a statement he had been contacted by the parents and agreed to speak with Charlie’s doctors to determine whether the experimental therapy he was developing could help improve the child’s condition).
The report says when Hirano traveled to London this month to examine Charlie, about six months after he had first been invited, a series of scans showed that the boy had suffered muscular atrophy, that the damage was irreversible and that treatment would be futile.
Yates criticised the hospital, saying it had dragged its feet about the treatment until it was too late. But, the report says, the hospital consistently stood by its contention that treatment would have been useless and that Charlie had irreversible brain damage. “If Charlie has had a relationship with the world around him since his best interests were determined, it has been one of suffering,” it said.
Dominic Wilkinson, a neonatologist and professor of medical ethics at Oxford University, said the case offered a tragic lesson about the risks of doctors’ offering uncertain hope to desperate parents. At the same time, he said, the case underscored the importance of mediation during a dispute about treatment, noting that the communication breakdown in the Gard case had all the attributes of a “messy divorce.”
“To let a child go is incredibly difficult, but it is also incredibly important,” he said. “It is heartbreaking, but we have to know when to say enough is enough.”
Truog said the parents’ legal battle had tapped into the health care debate in the US, and was being seized upon by some to affirm a money-driven system in which patients who have the means can pursue experimental treatments, even if the chances of success are slim. But he said experimental treatments must be weighed against the benefits for society as a whole.
In the US, “no one can demand nonbeneficial treatments simply by claiming they are paying out of pocket,” he wrote in a recent article on the Gard case. “It would be extremely rare for a hospital in the US to admit patients for the exclusive purpose of receiving homeopathic therapy or unproven stem cell infusions,” he wrote, “regardless of how much the patient paid.”
Professor Julian Savulescu, director of the Oxford Uehiro Centre for Practical Ethics, explores about the ethical lessons we can take from this tragic tale.
Savulescu writes: "At some point in all of our lives, we have to let go. One can only admire Connie Yates and Chris Gard who fought so hard for Charlie. However, we should continue to question the original decision, and the way in which these decisions are made. Even if it is too late for Charlie now, we should improve how we make these decisions for the future.
“Back in January, there was an option for a trial of treatment that had some chance of success, a world leading doctor willing and able to provide it, and, by April, the funds had been raised to achieve it without public funds.
“There were also the means to control and minimise Charlie's suffering. I believe that a limited trial of treatment was in Charlie’s interests back then, given the only alternative for him was death.
“Doctors opposed this because of the low chance of success combined with fears that the extra time in life support would be too painful.
“Four months of the legal process has left us with no trial of treatment, and no chance now for Charlie. Yet Charlie had to go through all the suffering (and more) of being kept alive on life support.
“No-one wanted this outcome. No-one believes this outcome was in Charlie’s best interests. There has got to be a better process. It has been traumatic for all the doctors, who have genuinely had Charlie's interests at heart, and Connie and Chris, but most of all Charlie.
“It has also raised other issues.
“Charlie would have been the first to receive this treatment and some have said it risked Charlie being used as a guinea pig. Medicine won't progress without experiment and innovation.
“Over the years processes have been developed to protect patients and ensure the best scientific results. Double blind placebo controlled trials are the gold standard. I have argued that, for rare and deadly diseases with no existing therapies, it is in the patient's interests to access potential treatments earlier and without placebo, provided they have a reasonable scientific basis.
“There is little to lose and much to gain for this group of patients, and the protections that are in place can cause more harm than good for them.
“A second issue is that social media has given power to the people. Over the five court hearings, Trump and the Pope, and thousands of others have weighed in. We have had to have these discussions about how and who should decide on what makes life worth living and what kinds of chances are worth taking.
“The question of who should decide is legitimate. Some people have wrongly concluded that these decisions should only be up to parents, but at the same time it is right that doctors, scientific experts and the Courts should not be considered almighty, beyond question or account.
“How much should the decision–making be left to parents? While most parents want to do the best for their children, parents can abuse their children, or can be radically mistaken. We do need oversight to ensure children are protected.
“If Connie Yates and Chris Gard had requested ongoing intensive care for a herbal treatment with zero scientific evidence or rationale, that would be abuse. But they weren't. They were asking for a treatment with a clear scientific rationale and some relevant evidence, with the support of a relevantly qualified medical expert.
“There have to be protections. But doctors should not activate these legal mechanisms, or stop parents travelling for medical care for their child, unless there is disagreement between the parents, or they are going to an unsafe place, or they are very confident the parents' choice is unreasonable.
“That requires doctors to think ethically, as well as having all the scientific evidence. The problem is not who has the power, it is how it is used and the need for robust, and humble, ethical deliberation.
“Some have seen this as a further attack on ‘experts’, a current hot topic. But this case was more about disputed values than disputed facts. What has been absent, and is absent from society, is a sound secular ethical approach to these life and death issues.
I haven't seen any substantial ethical discussion of the deep ethical issues in this case like what makes a life worth living or what kinds of chance are worth taking.
“Debate has been shut down in monosyllabic ethical argument: treatment is futile or it is not futile. And we have again closed our eyes to the elephant in the room: resources and justice. The NHS may not be able to afford such experimental treatments for everyone who needs them.
“We should have had a debate about resources and justice. These are difficult questions but ones that must be addressed openly. It goes beyond accepting the expertise of someone else.
“This has been a clash of medicine, science, politics, ethics and religion. Yes, there is always a clash of values because many people hold different values and weigh facts differently. What matters is that people's values are reasonable and they don't seek to impose them on others, or other families.
“It would have been very reasonable for Charlie's parents to choose to withdraw treatment; it was also very reasonable to choose a small chance of some improvement. I wouldn't choose experimental treatment if I were Charlie's parents but that does not mean they are wrong or unreasonable to do so.
“We need a bit of humility about our moral views about the good life, and about how and when to live. In Charlie's case, his parents have been accused of prioritising their own interests over Charlie's in choosing to take their child for experimental treatment that might give him a chance to live.
“The courts have intervened and stopped them. However, it is a reasonable view of Charlie’s interests that his parents held. I hope that there will be a review of the basis of these decisions, and how they are decided in the light of this case."
[link url="https://www.nytimes.com/2017/07/28/world/europe/charlie-gard-dead.html?emc=edit_th_20170729&nl=todaysheadlines&nlid=42505380"]The New York Times report[/link]
[link url="http://jamanetwork.com/journals/jama/fullarticle/2645763"]JAMA article[/link]
[link url="http://www.ox.ac.uk/news/arts-blog/ethical-legacy-charlie-gard-case"]University of Oxford material[/link]
