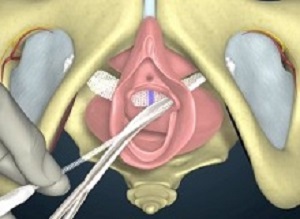
 Many more women than initially estimated who received vaginal mesh implants to treat incontinence will need the procedure reversed, a large study from the London School of Hygiene and Tropical Medicine found.
Many more women than initially estimated who received vaginal mesh implants to treat incontinence will need the procedure reversed, a large study from the London School of Hygiene and Tropical Medicine found.
In a study of nearly 100,000 English women, 3,137 (3.3%) required the implant to be removed within a decade. This is a third larger than the number of reversals reported in an NHS audit of the procedure. NHS England estimated just 2.6% had to be removed because of complications, but the rate may be even higher for younger women as 4.4% of those aged 18 to 39 had a removal.
Researchers from the London School of Hygiene and Tropical Medicine found that overall, 6.9% of women who had the procedure needed a further operation, but the reasons why were not recorded.
Dr Lucia Dolan, co-author of the study and consultant gynaecologist is quoted in the report as saying: “Women undergo tape removal when a complication has occurred. “There are no temporary mesh procedures – the expectation is that they are permanent. Unfortunately, many women who have mesh tapes removed will experience incontinence again.”
Urinary incontinence will affect one in three women at some point in their lives, but mesh implants commonly used to treat the condition have been linked to life-changing side effects.
The report says mesh implants have been the subject of law suits involving thousands of women in the US, UK and elsewhere who have been left with injuries when their implants deform, lacerating soft tissues of the vaginal canal and causing pain and disability.
In England NHS, trusts were told the devices should be a “last resort” and should only be implanted under “high vigilance”. This requires all doctors who perform the procedure to be experienced in using the devices and all patients to be regularly followed up with to ensure any side effects are reported.
The report says while rigid mesh implants used to treat organ prolapse after childbirth have been linked to the most acute side effects, the flexible mesh tapes more widely used to treat incontinence – and thought to be safer – have also been called in to question.
An NHS England estimate found that 500 mesh removal operations were taking place each year because of complications. Between 2008 and 2017 the NHS audit found 2,639 mesh tape removals among the 100,516 women who had the implants for stress incontinence.
But, the report says, the latest findings suggest it could be even higher. Based on NHS medical records for 95,000 women in England who had mesh implants between 2006 and 2015, more than 3,000 had a removal.
The authors note that the gradual decrease in mesh operations – falling 50% over this period – is “likely to reflect concerns about longer-term complications, outcomes, and risk of further surgery after (mesh) insertion”.
Abstract
Importance: There is concern about outcomes of midurethral mesh sling insertion for women with stress urinary incontinence. However, there is little evidence on long-term outcomes.
Objective: To examine long-term mesh removal and reoperation rates in women who had a midurethral mesh sling insertion for stress urinary incontinence.
Design, Setting, and Participants: This population-based retrospective cohort study included 95 057 women aged 18 years or older who had a first-ever midurethral mesh sling insertion for stress urinary incontinence in the National Health Service hospitals in England between April 1, 2006, and December 31, 2015. Women were followed up until April 1, 2016.
Exposures: Patient and hospital factors and retropubic or transobturator mesh sling insertions.
Main Outcomes and Measures: The primary outcome was the risk of midurethral mesh sling removal (partial or total) and secondary outcomes were reoperation for stress urinary incontinence and any reoperation including mesh removal, calculated with death as competing risk. A multivariable Fine-Gray model was used to calculate subdistribution hazard ratios as estimates of relative risk.
Results: The study population consisted of 95 057 women (median age, 51 years; interquartile range, 44-61 years) with first midurethral mesh sling insertion, including 60 194 with retropubic insertion and 34 863 with transobturator insertion. The median follow-up time was 5.5 years (interquartile range, 3.2-7.5 years). The rate of midurethral mesh sling removal was 1.4% (95% CI, 1.3%-1.4%) at 1 year, 2.7% (95% CI, 2.6%-2.8%) at 5 years, and 3.3% (95% CI, 3.2%-3.4%) at 9 years. Risk of removal declined with age. The 9-year removal risk after transobturator insertion (2.7% [95% CI, 2.4%-2.9%]) was lower than the risk after retropubic insertion (3.6% [95% CI, 3.5%-3.8%]; subdistribution hazard ratio, 0.72 [95% CI, 0.62-0.84]). The rate of reoperation for stress urinary incontinence was 1.3% (95% CI, 1.3%-1.4%) at 1 year, 3.5% (95% CI, 3.4%-3.6%) at 5 years, and 4.5% (95% CI, 4.3%-4.7%) at 9 years. The rate of any reoperation, including mesh removal, was 2.6% (95% CI, 2.5%-2.7%) at 1 year, 5.5% (95% CI, 5.4%-5.7%) at 5 years, and 6.9% (95% CI, 6.7%-7.1%) at 9 years.
Conclusions and Relevance: Among women undergoing midurethral mesh sling insertion, the rate of mesh sling removal at 9 years was estimated as 3.3%. These findings may guide women and their surgeons when making decisions about surgical treatment of stress urinary incontinence.
Authors
Ipek Gurol-Urganci; Rebecca S Geary; Jil B Mamza; Jonathan Duckett; Dina El-Hamamsy; Lucia Dolan; Douglas G Tincello; Jan van der Meulen
[link url="https://www.independent.co.uk/news/health/vaginal-mesh-implant-urinary-incontinence-women-pain-disability-lawsuit-nhs-a8597956.html"]The Independent report[/link]
[link url="https://jamanetwork.com/journals/jama/article-abstract/2708113"]JAMA abstract[/link]
