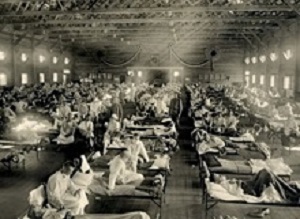
Dr Stefan E Pambuccian, a Loyola Medicine cytologist, surgical pathologist and professor and vice chair of the department of pathology and laboratory medicine at Loyola University Chicago Stritch School of Medicine, has reviewed published data and research from three papers dating back to the 1918-19 Spanish flu pandemic, which infected one-fifth to one-third of the world's population and killed 50m people.
According to the data and analysis, cities that adopted early, broad isolation and prevention measures – closing of schools and churches, banning of mass gatherings, mandated mask wearing, case isolation and disinfection/hygiene measures – had lower disease and mortality rates. These cities included San Francisco, St Louis, Milwaukee and Kansas City, which collectively had 30% to 50% lower disease and mortality rates than cities that enacted fewer and later restrictions. One analysis showed that these cities also had greater delays in reaching peak mortality, and the duration of these measures correlated with a reduced total mortality burden.
"The stricter the isolation policies, the lower the mortality rate," says Pambuccian. He studied the Spanish flu, including prevention measures and outcomes, to help develop standards for staffing and safety in the cytology lab, where infectious diseases like the COVID-19 virus are diagnosed and studied at the cellular level.
Like today, not everyone in 1918 and 1919 thought the strict measures were appropriate or effective at the time. An estimated 675,000 people died in the US from the Spanish flu, "and there was scepticism that these policies were actually working," says Pambuccian. "But they obviously did make a difference."
In 1918, the world was still at war "with overcrowded barracks," and much of the US lived with "poverty, poor nutrition, poor hygiene, household/community-level crowding, and a lack of preparation of the population and decision makers due to cognitive inertia and poor medical and insufficient nursing care," says Pambuccian.
"Although the world is a much different place than it was 100 years ago, the efficacy of the measures instituted during the 1918-19 pandemic gives us hope that the current measures will also limit the impact of the COVID-19 pandemic."
Abstract
The coronavirus disease 2019 (COVID-19) is a pandemic with the SARS-CoV-2 virus. The infection has predominantly respiratory transmission and is transmitted through large droplets or aerosols, and less commonly by contact with infected surfaces or fomites. The alarming spread of the infection and the severe clinical disease that it may cause, have led to the widespread institution of social distancing measures. Due to repeated exposure to potentially infectious patients and specimens, healthcare and laboratory personnel are particularly susceptible to contract COVID-19. This review paper provides an assessment of the current state of knowledge about the disease and its pathology, and the potential presence of the virus in cytology specimens. It also discusses the measures that cytology laboratories can take to function during the pandemic, and minimize the risk to their personnel, trainees and pathologists. In addition, it explores potential means to continue to educate trainees during the COVID-19 pandemic.
Authors
Stefan E Pambuccian
[link url="https://www.sciencedaily.com/releases/2020/03/200330110344.htm"]Loyola University Health System material[/link]
[link url="https://www.sciencedirect.com/science/article/pii/S2213294520300454?via%3Dihub"]Journal of the American Society of Cytopathology abstract[/link]