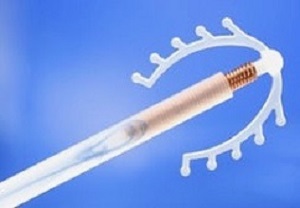
 Considered a safe and highly effective contraception method, intrauterine devices (IUDs) may also be quietly offering protection against the third-most common cancer in women worldwide. A new study from the Keck School of Medicine of the University of Southern California has found that IUD use is associated with a dramatic decrease in the incidence of cervical cancer.
Considered a safe and highly effective contraception method, intrauterine devices (IUDs) may also be quietly offering protection against the third-most common cancer in women worldwide. A new study from the Keck School of Medicine of the University of Southern California has found that IUD use is associated with a dramatic decrease in the incidence of cervical cancer.
The systematic review is the first to combine data from multiple studies on IUDs and cervical cancer. The analysis included data from 16 high-quality observational studies involving more than 12,000 women worldwide. Results showed that in women who used an IUD, the incidence of cervical cancer was a third lower.
“The pattern we found was stunning. It was not subtle at all,” says the study’s lead author, Dr Victoria Cortessis, associate professor of clinical preventive medicine at the Keck School. “The possibility that a woman could experience some help with cancer control at the same time she is making contraception decisions could potentially be very, very impactful.”
The number of women diagnosed with cervical cancer is steadily rising. According to the World Health Organisation (WHO), approximately 528,000 women were diagnosed with cervical cancer worldwide in 2012, and 266,000 women died from the disease. By 2035, the WHO projects that those numbers will climb to more than 756,000 and 416,000, respectively.
For women in developing countries, where cervical cancer prevention resources such as the human papillomavirus (HPV) vaccine or regular cervical screenings are scarce, and where populations are increasing rapidly, a contraceptive that offers protection against cervical cancer could have a profound effect, Cortessis explains.
“A staggering number of women in the developing world are on the verge of entering the age range where the risk for cervical cancer is the highest – the 30s to the 60s. Even if the rate of cervical cancer remains steady, the actual number of women with cervical cancer is poised to explode,” Cortessis says. “IUDs could be a tool to combat this impending epidemic.”
Should gynaecologists begin recommending IUDs for protection against cervical cancer?
Not quite yet, but it could be on the horizon. Understanding the mechanism of action behind the protective effect of IUDs is the next logical step, Cortessis says. Some scientists speculate that the placement of an IUD stimulates an immune response in the cervix, giving the body an opportunity to fight an existing HPV infection that could one day lead to cervical cancer. Another possibility is that when an IUD is removed, some cervical cells that contain HPV infection or precancerous changes may be scraped off.
“If we can demonstrate that the body mounts an immune response to having an IUD placed, for example, then we could begin investigating whether an IUD can clear a persistent HPV infection in a clinical trial,” explains gynecologic oncologist and study co-author Laila Muderspach, chair of obstetrics and gynaecology at the Keck School. “The results of our study are very exciting. There is tremendous potential.”
Abstract
Objective: To estimate the association between use of an intrauterine device (IUD) and risk of cervical cancer by subjecting existing data to critical review, quantitative synthesis, and interpretation.
Data Soruces: We searched PubMed, Web of Science, ClinicalTrials.gov, and catalogs of scientific meetings and abstracts, theses, and dissertations queried from inception through July 2016.
Methods of Study Selection: Examination of abstracts from 225 reports identified 34 studies with individual-level measures of use of an IUD and incident cervical cancer. By critically assessing the full text of these reports, independent reviewers identified 17 studies conducted without recognized sources of systematic error, of which 16 could be harmonized for meta-analysis.
Tabulation, Integration and Results: Point and interval estimates of the association between use of an IUD and incident cervical cancer were extracted from original reports into a structured database along with key features of study design and implementation. A random-effects meta-analysis was implemented to quantitatively synthesize extracted estimates and assess likely influence of publication bias, residual confounding, heterogeneity of true effect size, and human papillomavirus prevalence and cervical cancer incidence in source populations. Women who used an IUD experienced less cervical cancer (summary odds ratio 0.64, 95% CI 0.53–0.77). Neither confounding by recognized risk factors nor publication bias seems a plausible explanation for the apparent protective effect, which may be stronger in populations with higher cervical cancer incidence.
Conclusion: Invasive cervical cancer may be approximately one third less frequent in women who have used an IUD. This possible noncontraceptive benefit could be most beneficial in populations with severely limited access to screening and concomitantly high cervical cancer incidence.
Authors
Cortessis, Victoria K; Barrett, Malcolm; Brown Wade, Niquelle; Enebish, Temuulen; Perrigo, Judith L; Tobin, Jessica; Zhong, Charlie; Zink, Jennifer; Isiaka, Vanessa; Muderspach, Laila I; Natavio, Melissa; McKean-Cowdin, Roberta
[link url="https://keck.usc.edu/iuds-cervical-cancer-protection/"]Keck School of Medicine material[/link]
[link url="http://journals.lww.com/greenjournal/Abstract/publishahead/Intrauterine_Device_Use_and_Cervical_Cancer_Risk_.98222.aspx"]Obstetrics & Gynaecology abstract[/link]
